How Your Vagus Nerve Detects and Fights Inflammation
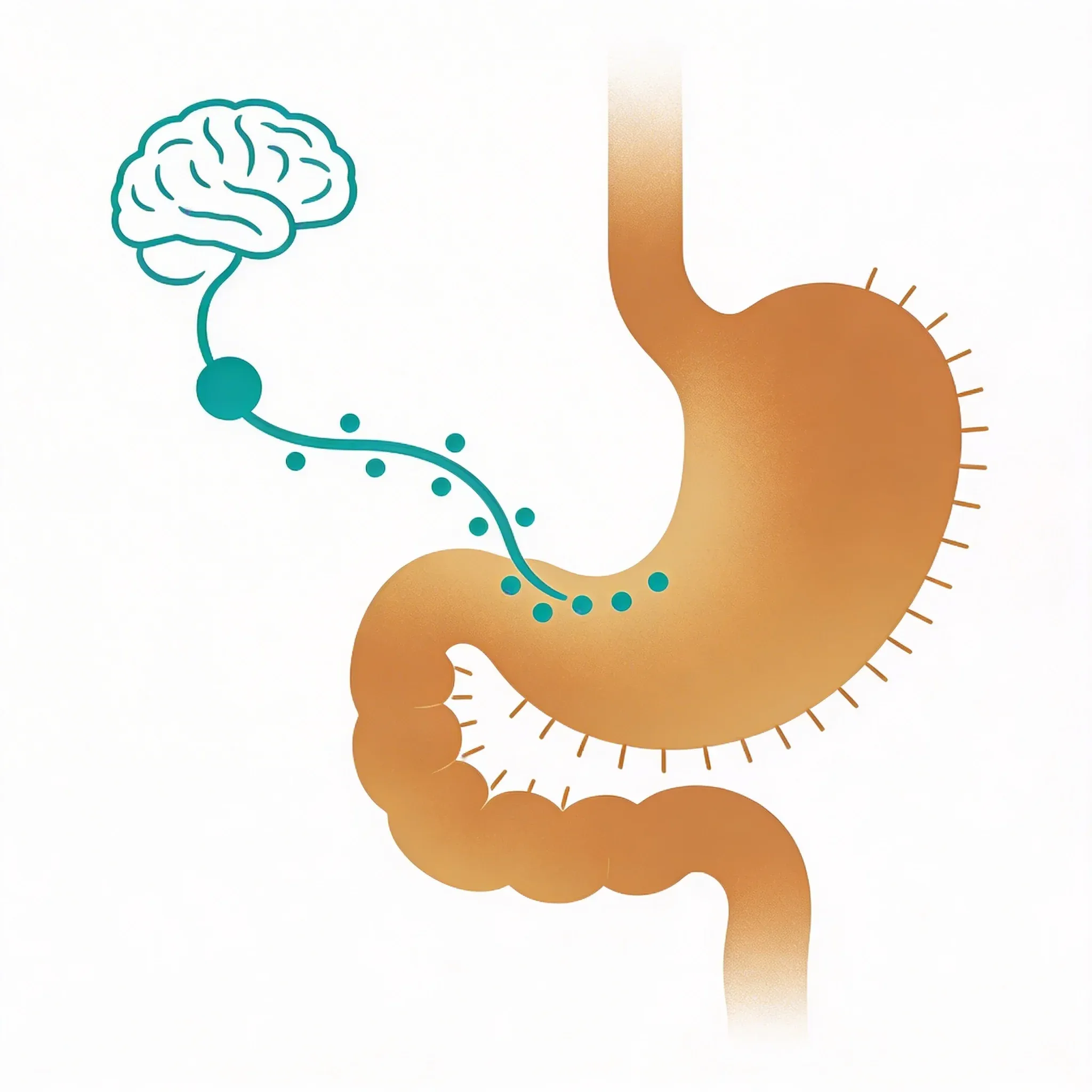
Your vagus nerve acts as a two-way highway between your brain and immune system. It can directly detect inflammatory signals called cytokines. It responds by releasing natural anti-inflammatory chemicals. This creates a feedback loop that helps prevent too much inflammation while keeping your body's ability to fight real threats1.
What Are Cytokines and Why Do They Matter?
Cytokines are tiny signaling proteins. Your immune cells release them when they detect trouble. Think of them as your body's text messages.
When you get injured or infected, immune cells flood the area. They start texting each other through cytokines. The main inflammatory messengers include TNF-alpha and IL-1β. These proteins basically yell "we have a problem!" throughout your system1.
But your body also makes anti-inflammatory cytokines like IL-10. These work like calming messages. They say "everything's under control now." The balance between pro and anti-inflammatory signals determines whether your immune response helps or hurts you.
Here's where it gets interesting:
Your vagus nerve can "read" these cytokine messages directly. It doesn't just carry signals from your brain down to your organs. It also picks up chemical information from your immune system and reports back upstairs.
How Does the Vagus Nerve Detect Inflammation?
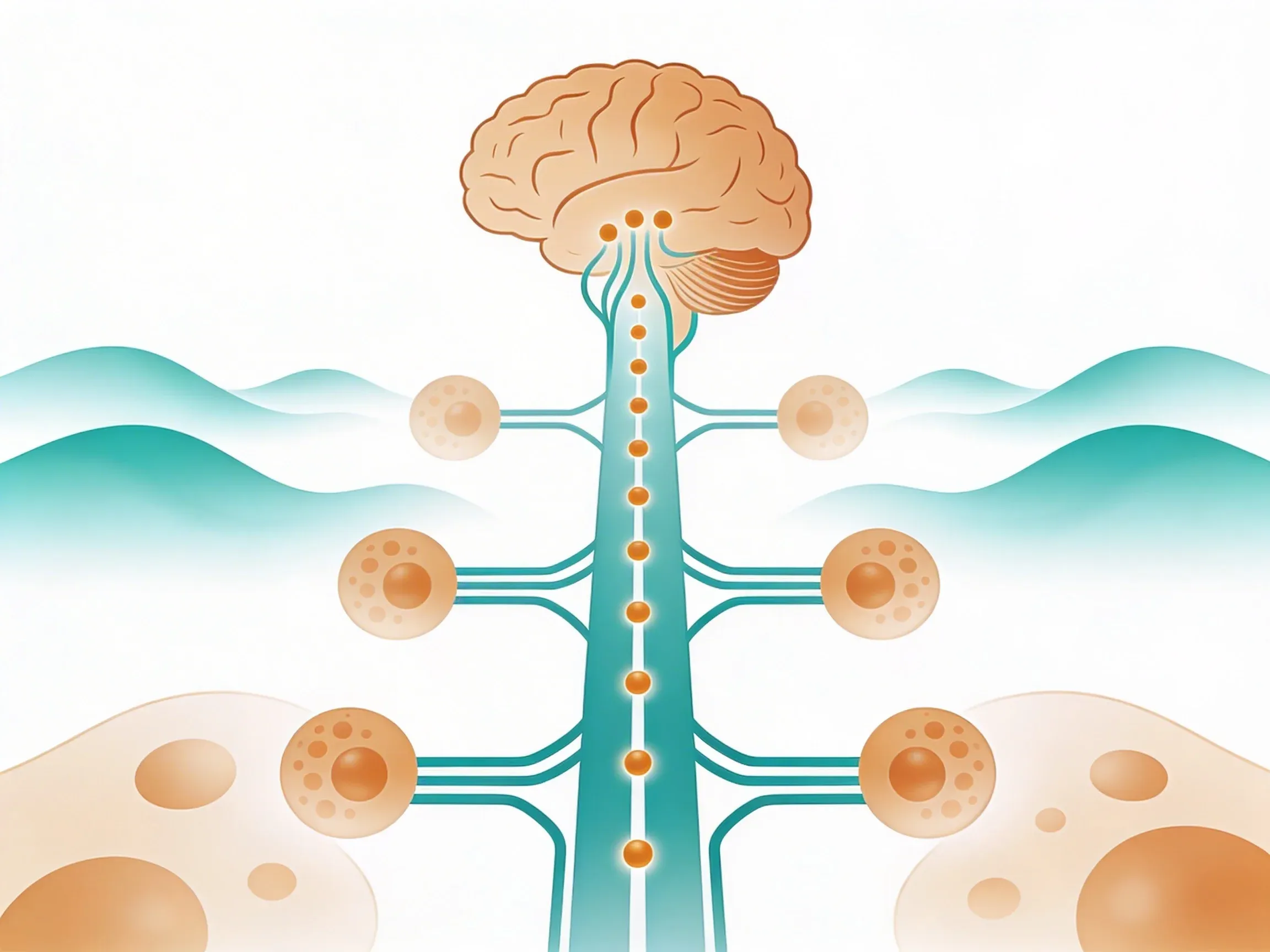
Your vagus nerve has special sensors called nodose ganglia neurons. These act like chemical detectors stationed along the nerve pathway.
When cytokines like TNF or IL-1β appear in your bloodstream or tissues, these vagal sensors bind to them directly. Each type of cytokine creates a unique electrical signature. It's like different ringtones for different types of inflammation2.
Once detected, the vagus nerve converts these chemical signals into electrical impulses. These travel up to your brainstem. They go to an area called the nucleus tractus solitarius. This brain region processes the immune information and decides how to respond.
Recent 2025 research in Nature Communications showed something amazing. Vagus nerve recordings can tell different cytokines apart based on their electrical patterns1. Your brain literally knows the difference between an allergic reaction and a bacterial infection. It uses vagal nerve signals to figure this out.
The whole detection process happens very fast. Within minutes of cytokine release, your brain knows what type of immune response is happening and where.
What Happens When Your Brain Receives Inflammation Signals?
Once your brain processes the cytokine information from your vagus nerve, it can respond in several ways.
First, it might trigger behavior changes. That sudden urge to rest when you're getting sick? That's your brain responding to inflammatory cytokines detected by your vagus nerve. The brain reads these signals as "time to save energy for healing."
Second, your brain can turn on the cholinergic anti-inflammatory pathway. This is where things get really clever.
Your brain sends signals back down the vagus nerve. This releases acetylcholine near immune cells. Acetylcholine acts like a "calm down" signal to overactive immune cells. It reduces their production of inflammatory cytokines3.
This creates a natural feedback loop. More inflammation triggers more vagus nerve activity. This releases more acetylcholine. This reduces inflammation. It's your body's built-in thermostat for immune responses.
How Does Vagal Tone Affect Cytokine Balance?
People with higher vagal tone tend to have lower levels of inflammatory cytokines in their blood4. Vagal tone is measured through heart rate variability.
This makes sense when you understand the mechanism. A more active vagus nerve means:
- Better detection of early inflammatory signals
- Faster anti-inflammatory responses
- More consistent acetylcholine release to calm immune cells
Research shows that people with higher HRV have lower levels of TNF-alpha and IL-6. These are two key inflammatory markers. They also recover faster from inflammatory challenges like intense exercise or mental stress.
The relationship works both ways. Long-term inflammation can actually hurt vagus nerve function over time. This creates a bad cycle. Poor vagal tone leads to more inflammation. This further reduces vagal tone.
That's why supporting vagus nerve health may help maintain better immune balance long-term.
Can You Improve Your Vagus Nerve's Inflammation Response?
While this describes natural body processes, certain practices may support healthy vagus-immune communication.
Slow, deep breathing appears to turn on the vagus nerve. It promotes relaxation responses. Some research suggests regular breathing exercises may help maintain healthy cytokine levels. But more studies are needed.
Cold exposure, moderate exercise, and good sleep also support vagal tone. These lifestyle factors may indirectly help your vagus nerve maintain better immune system communication.
Some people explore vagus nerve stimulation devices. They use these as a way to support this natural anti-inflammatory pathway. While the research is promising, it's still emerging.
The key insight is this: your vagus nerve and immune system are in constant conversation. Supporting this communication system may help your body maintain the delicate balance. It needs to fight threats while preventing harmful inflammation.