Do you wake up feeling stiff and achy? Does that afternoon energy crash hit like clockwork? These everyday symptoms might be signs that chronic inflammation is quietly working against you. The good news? Your body has a built-in system to fight inflammation -- the cholinergic anti-inflammatory pathway. This network uses your vagus nerve to tell immune cells when to dial down inflammation. Through specific breathing techniques, targeted foods, and simple daily practices, you can activate this natural system to help reduce chronic inflammation throughout your body.
How Does Your Vagus Nerve Control Inflammation?
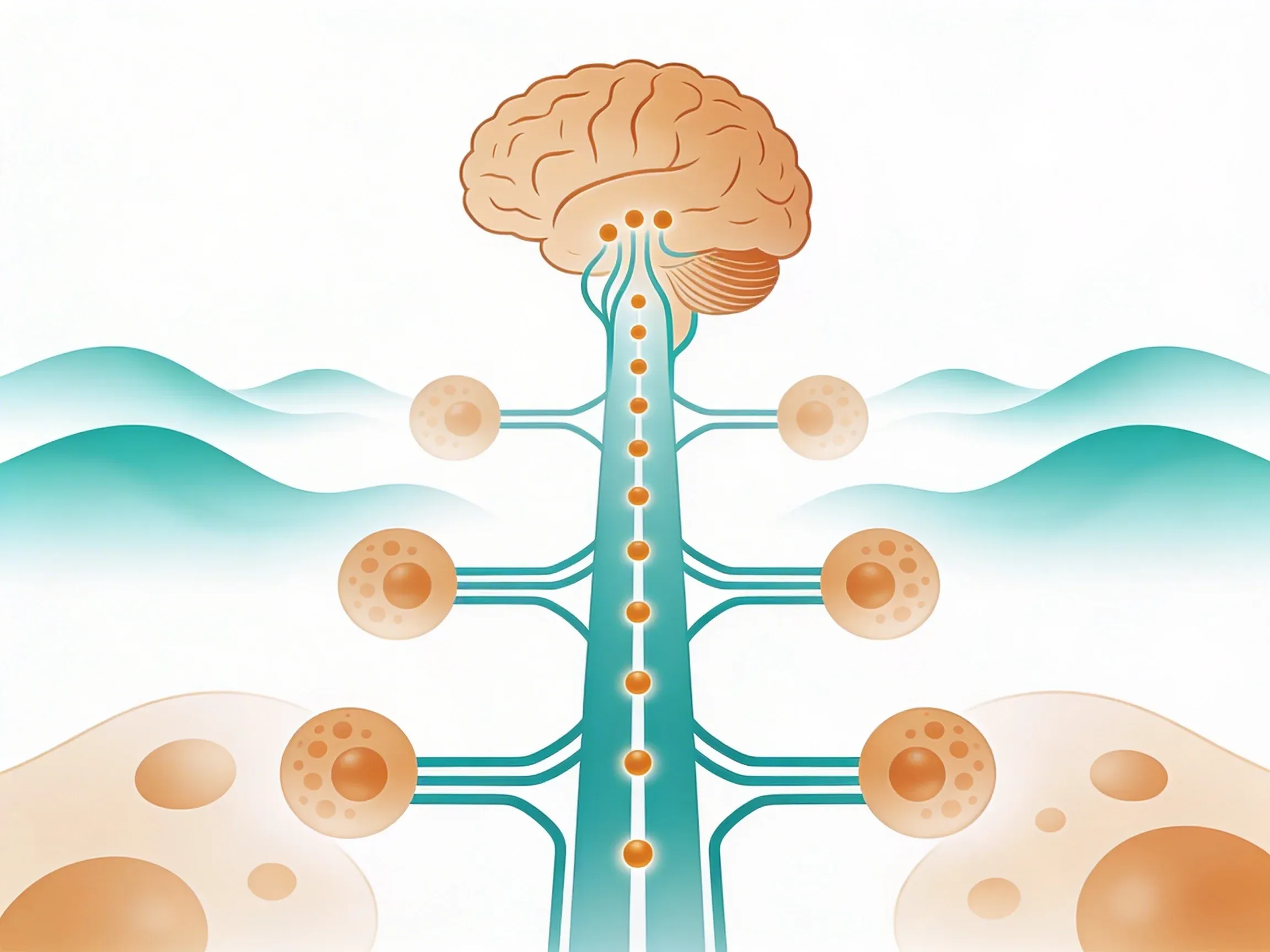
Think of your vagus nerve as a communication highway between your brain and immune system. When it's working well, this nerve releases acetylcholine -- like traffic signals that tell immune cells when to slow down and reduce their production of inflammatory compounds like cytokines. Without these chemical signals, your white blood cells keep producing inflammation even when the threat is gone.
Here's the thing: chronic stress and poor lifestyle habits can weaken this pathway. When your anti-inflammatory system gets overwhelmed, it contributes to the low-grade inflammation linked to heart disease, diabetes, and other chronic conditions.
But you can strengthen it. Recent research shows that vagus nerve stimulation can regulate key inflammation pathways, including NF-κB and NLRP31. These are the molecular switches that control how much inflammation your body produces. Now let's explore specific ways to strengthen this natural system.
Can Breathing Exercises Actually Reduce Inflammation?
Slow, controlled breathing is one of the fastest ways to activate your vagus nerve's anti-inflammatory response. When you breathe deeply and slowly, you stimulate the nerve fibers that run through your diaphragm.
Try this: breathe in for 4 counts, hold for 2, then exhale slowly for 8 counts. The long exhale is key -- it activates your parasympathetic nervous system and triggers acetylcholine release.
Studies suggest that people who practice regular breathing exercises show measurable changes in inflammatory markers. The effect isn't instant, but most people notice improvements in how they feel within 2-3 weeks of consistent practice.
For maximum benefit, aim for 5-10 minutes of slow breathing daily. You can do this anywhere -- during your commute, before bed, or when you need to shift into calm mode.
What Foods Best Support Your Anti-Inflammatory Pathways?
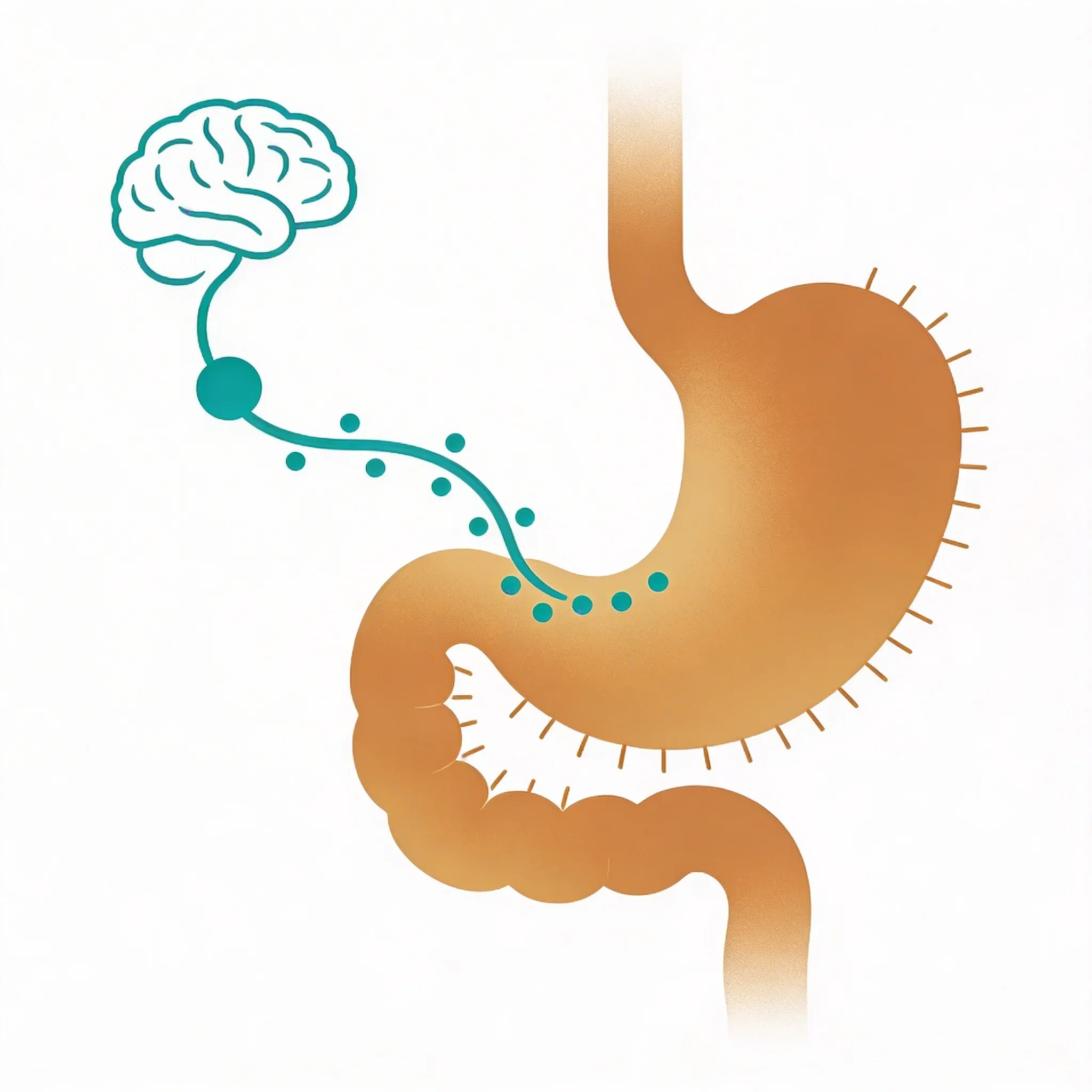
Certain foods directly support the cholinergic anti-inflammatory pathway. Your gut and brain are connected through the vagus nerve, so what you eat influences how well this system works.
Omega-3 rich fish like salmon, sardines, and mackerel provide the building blocks for anti-inflammatory compounds. Aim for 2-3 servings per week.
Colorful vegetables contain phytochemicals that support vagal function. Beets are particularly powerful -- they contain betaine, an antioxidant that helps reduce inflammatory markers2.
Fermented foods like yogurt, kefir, and sauerkraut feed beneficial gut bacteria. A healthy microbiome communicates with your vagus nerve to maintain balanced inflammation responses.
Avoid processed foods, excess sugar, and trans fats. These trigger inflammatory pathways and can interfere with your vagus nerve's ability to regulate immune responses.
How Does Stress Management Activate Anti-Inflammatory Responses?
Chronic stress is inflammation's best friend. When you're constantly stressed, your brain's alarm center (the amygdala) overrides your vagus nerve's calming signals.
Your prefrontal cortex -- the thinking, planning part of your brain -- can help counter this. When you practice mindfulness, meditation, or even gentle exercise, you strengthen the connection between your thinking brain and your vagus nerve.
This isn't just feel-good advice. Research shows that people who manage stress well have lower levels of inflammatory markers in their blood. They also show better heart rate variability, a sign that their vagus nerve is functioning optimally.
Start small: even 5 minutes of meditation or a 10-minute walk can help reset your nervous system.
Which Daily Practices Strengthen Your Anti-Inflammatory System?
Building anti-inflammatory habits doesn't require major lifestyle overhauls. Small, consistent actions compound over time.
Cold exposure activates your vagus nerve through the dive reflex. A 30-second cold shower or splash of cold water on your face triggers this response. Start with just a few seconds and build up gradually.
Gentle movement like yoga, tai chi, or walking supports vagal tone while reducing stress hormones. The key is consistency, not intensity.
Quality sleep gives your anti-inflammatory pathways time to reset. Poor sleep disrupts vagus nerve function and increases inflammatory markers. Aim for 7-9 hours nightly.
Social connection also matters. Positive relationships reduce stress and support healthy vagal function. Even brief, meaningful interactions can help activate your body's anti-inflammatory responses.
The bottom line? Your body wants to maintain balanced inflammation. By supporting your vagus nerve through breathing, nutrition, and stress management, you're working with your natural systems rather than against them.