Your vagus nerve acts as a natural brake on your immune system, releasing acetylcholine to calm excessive inflammation and help your body fight infections more effectively. Higher vagal tone -- often measured through heart rate variability -- is linked to better immune regulation and reduced risk of chronic inflammatory conditions1.
What Is the Cholinergic Anti-Inflammatory Pathway?
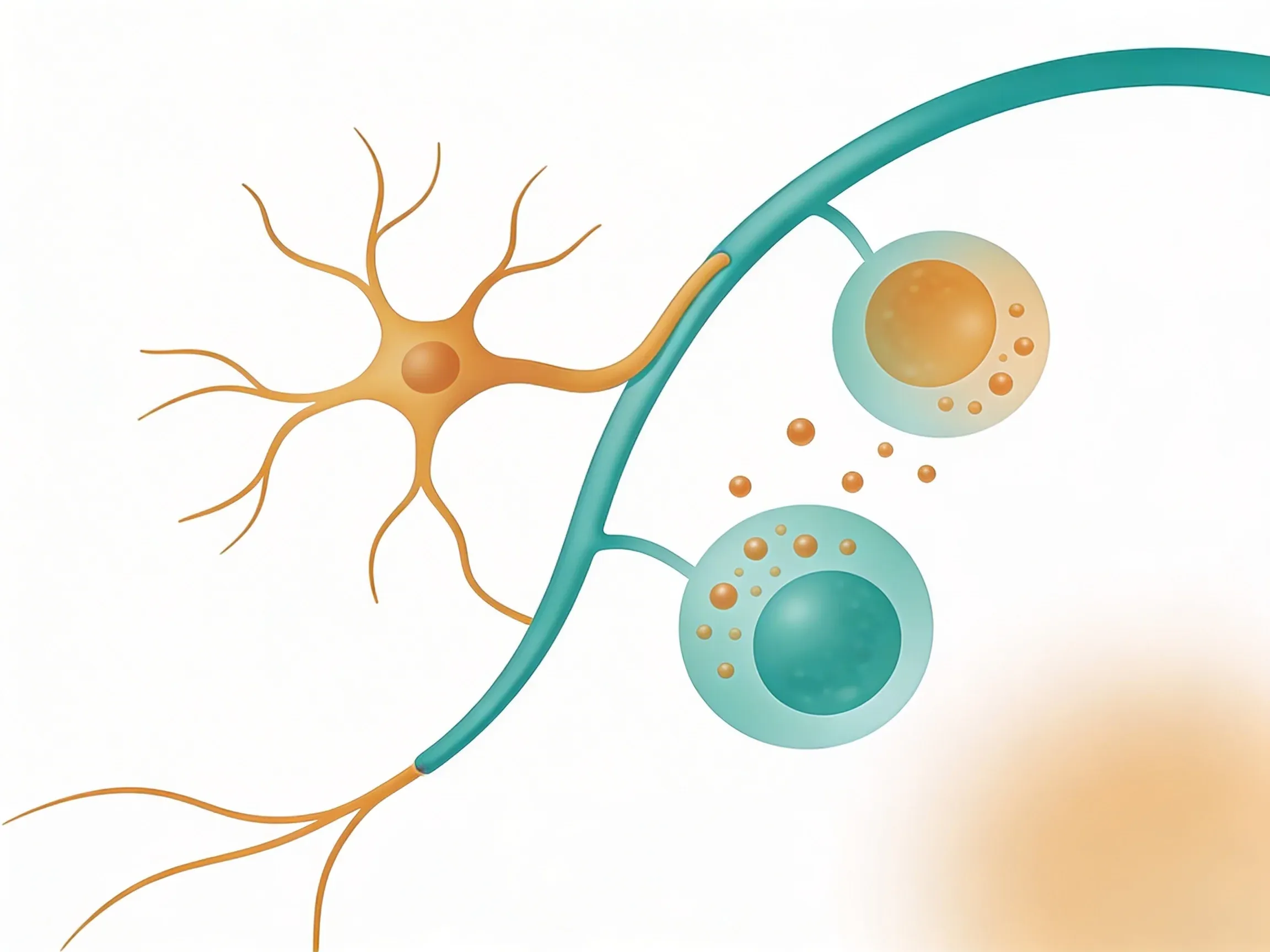
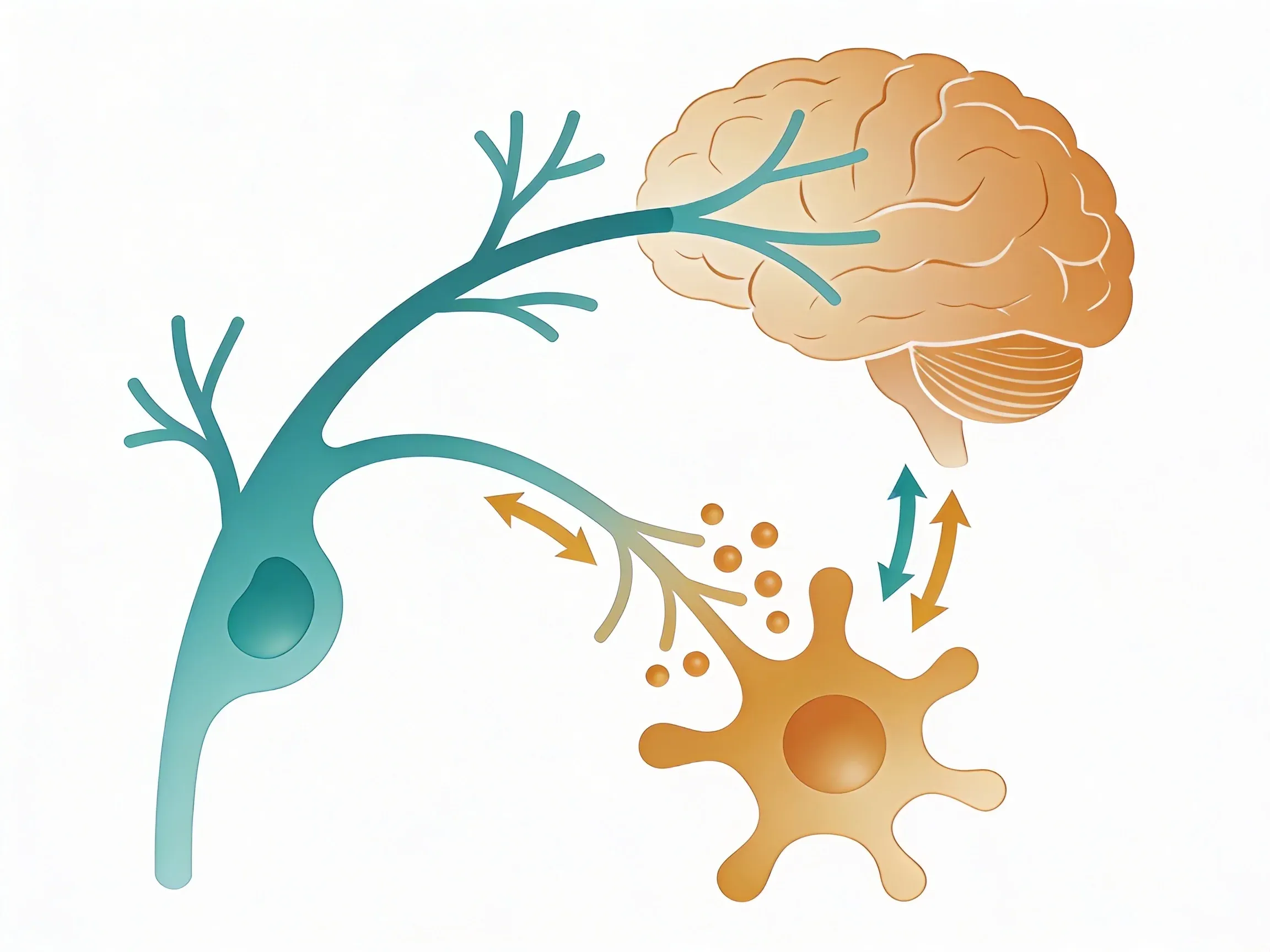
Think of your vagus nerve as your immune system's wise counselor. When infection or injury triggers inflammation, your immune cells start pumping out inflammatory signals called cytokines. That's good -- you need inflammation to heal.
But sometimes your immune system gets carried away. It keeps firing long after the threat is gone. That's where your vagus nerve steps in.
The vagus nerve releases a chemical messenger called acetylcholine. This molecule tells overactive immune cells to dial it back. It specifically targets cells that produce tumor necrosis factor (TNF) and other pro-inflammatory cytokines2. The result? Your body can still fight threats, but it doesn't attack itself in the process.
This system is so important that researchers call it the "cholinergic anti-inflammatory pathway". It's your body's built-in way to prevent inflammation from spiraling out of control.
How Does Vagal Tone Affect Your Immune Response?
People with higher vagal tone tend to have more balanced immune systems. Their bodies are better at ramping up immune responses when needed and shutting them down when the job is done.
Here's what happens when your vagal tone is strong:
Faster inflammation resolution. Your immune system can shift from "attack mode" to "repair mode" more quickly. This means less lingering inflammation after you recover from illness or injury.
Better regulatory T-cell production. Research shows vagus nerve stimulation can increase these specialized immune cells that help maintain balance and prevent your immune system from attacking healthy tissue1.
More precise immune responses. Instead of a whole-body inflammatory storm, your vagus nerve helps create targeted, localized responses. This saves energy and reduces collateral damage to healthy tissues.
The connection runs both ways. Chronic inflammation can also impair vagus nerve function, creating a cycle where poor immune regulation leads to even weaker vagal tone.
Can You Measure Immune Resilience Through HRV?
Heart rate variability (HRV) serves as a window into your vagal tone -- and potentially your immune health. When your HRV is higher, it often means your vagus nerve is firing well and keeping your nervous system balanced.
Some research suggests people with higher HRV tend to have:
- Better responses to vaccines
- Faster recovery from infections
- Lower markers of chronic inflammation
But here's the catch: HRV reflects many factors beyond just immune function. Stress, sleep, fitness, and even what you ate for lunch all influence your HRV readings.
So while HRV can give you clues about your overall resilience, it's not a direct measure of immune strength. Think of it as one piece of a bigger puzzle.
What Happens When Vagal Tone Is Low?
Many inflammatory and autoimmune conditions show up alongside reduced vagal function. People with conditions like rheumatoid arthritis, inflammatory bowel disease, and chronic fatigue often have lower HRV and signs of autonomic dysfunction3.
This doesn't mean low vagal tone causes these conditions. The relationship is complex. But it suggests that supporting vagal health might help some people manage inflammatory symptoms.
When vagus nerve fibers are damaged or not working well, they can't release enough acetylcholine to properly regulate immune responses. The result? Inflammation that lingers longer than it should and immune systems that struggle to find balance.
Can Improving Vagal Tone Support Immune Health?
The research is promising but still developing. Most studies on vagus nerve stimulation and immune function have used surgical implants or experimental settings -- not the kind of approaches most people can try at home.
That said, many of the practices that support vagal tone may also benefit immune health:
Structured breathing exercises activate your parasympathetic nervous system and may help shift your body toward the "rest and digest" state where healing happens. Try 4-7-8 breathing (inhale for 4 counts, hold for 7, exhale for 8) for 3-5 cycles before bed, or box breathing (4 counts in, hold for 4, out for 4, hold for 4) for 10-15 minutes daily.
Cold exposure triggers the dive reflex, which stimulates vagal activity. Beginners can start with 30-60 seconds of cold shower at 60-70°F (15-21°C) water temperature. More experienced practitioners may work up to 2-3 minutes at 50-60°F (10-15°C). Some people report feeling more resilient to minor illnesses after starting cold exposure routines.
Regular aerobic exercise supports both HRV and immune function. Aim for moderate-intensity activities like brisk walking, swimming, or cycling for 150 minutes per week (as recommended by health guidelines). Low-intensity yoga and tai chi practiced 2-3 times weekly may also specifically benefit vagal tone through their combination of movement, breathing, and relaxation.
Some people use vagus nerve stimulation devices as part of their wellness routine, though more research is needed to understand their effects on immune function specifically.
The bottom line? While we can't yet say definitively that improving vagal tone will boost your immune system, the early research points in that direction.