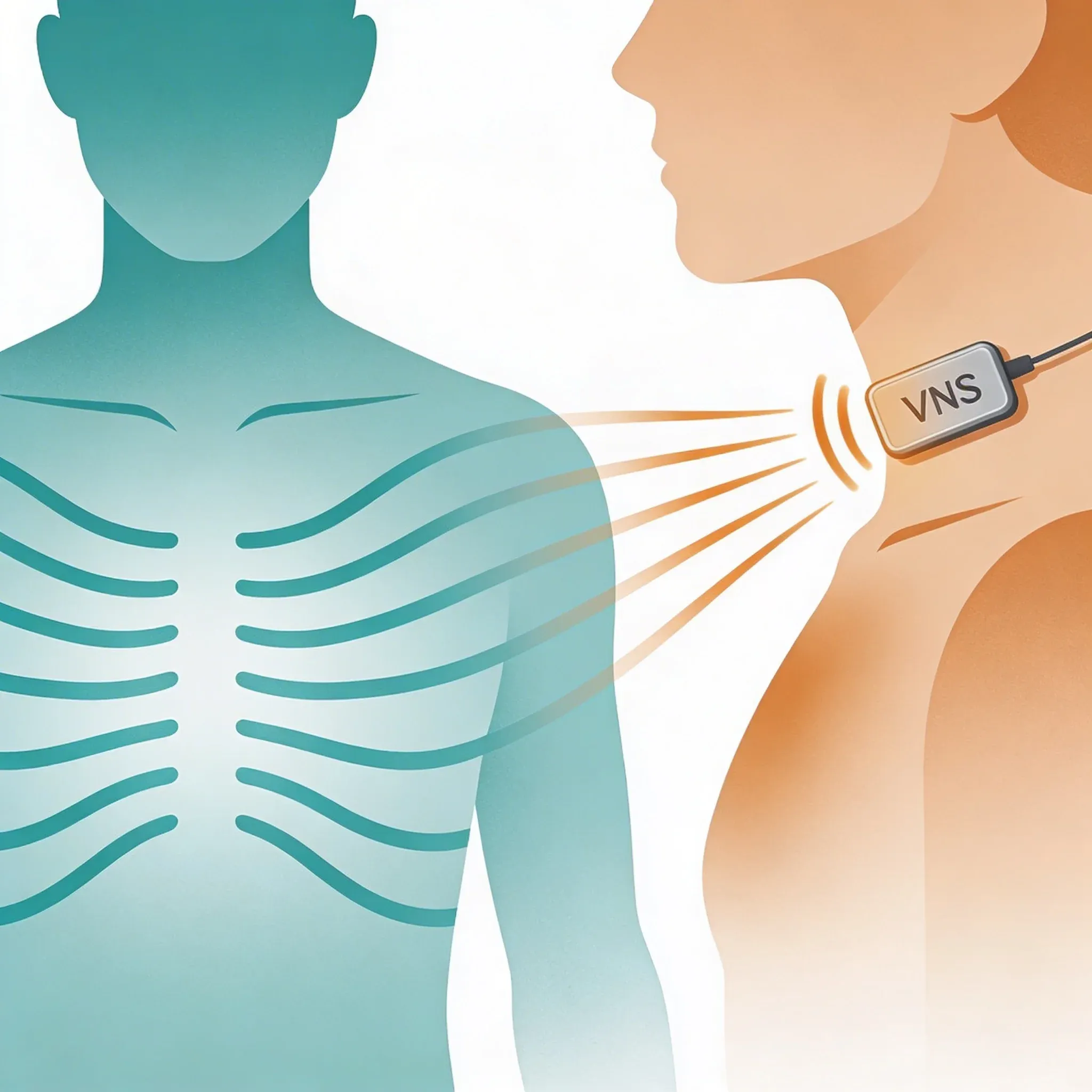
Vagus nerve stimulation may help reduce the rapid heart rate, dizziness, and fatigue that some people experience when standing up. Early studies show that transcutaneous vagus nerve stimulation (tVNS) can improve these symptoms within 2 months of treatment, particularly for people with postural orthostatic tachycardia syndrome (POTS)1.
What Happens When Standing Makes You Feel Awful?
For most people, standing up is no big deal. Your body automatically adjusts your heart rate and blood pressure to keep blood flowing to your brain.
But some people experience orthostatic intolerance. That's when standing triggers symptoms like:
- Heart rate jumping 30+ beats per minute
- Dizziness or lightheadedness
- Fatigue that hits like a wall
- Brain fog or trouble thinking clearly
- Nausea or stomach discomfort
This happens when your autonomic nervous system -- the part that controls automatic body functions -- doesn't respond properly to position changes. Your sympathetic nervous system (fight-or-flight mode) goes into overdrive. Meanwhile, your parasympathetic system (rest-and-digest mode) stays too quiet.
The result? Your body acts like you're in danger when you're just trying to stand up.
How Does Vagus Nerve Stimulation Address Standing Intolerance?
Your vagus nerve is the main highway for your parasympathetic nervous system. When it's working well, it helps balance out that overactive fight-or-flight response.
Here's the thing: people with orthostatic intolerance often have weakened vagal tone. Their vagus nerve isn't firing strongly enough to counteract the sympathetic overdrive.
Transcutaneous vagus nerve stimulation works by sending gentle electrical pulses through the skin to activate this nerve. Research suggests tVNS helps restore what scientists call "sympathovagal balance" -- basically, it strengthens the calm-down signals to match the revved-up ones2.
Think of it like adding weight to the quiet side of a see-saw that's been stuck tilted toward panic.
What Does the Research Show About VNS for Standing Problems?
The research is still early, but the results look promising. Most studies have focused on people with POTS, the most common form of orthostatic intolerance.
A randomized controlled trial found that people using tVNS for 2 months saw significant improvement in their orthostatic tachycardia compared to those using a sham device1. That means their heart rate didn't spike as much when they stood up.
Even single sessions of tVNS have shown benefits. Short-term studies found that one treatment session could reduce excessive heart rate jumps and lower overall symptom scores when people stood up2.
But there's a catch.
Most of this research involves small groups of people -- we're talking dozens, not hundreds or thousands. And the studies are short-term. We don't yet know how well VNS works long-term or for people with other types of standing intolerance beyond POTS.
How Might VNS Work for Orthostatic Symptoms?
Researchers think tVNS helps orthostatic intolerance through several pathways:
Anti-adrenergic effects: It may dial down the excessive adrenaline response that makes your heart race when you stand. Less adrenaline means less of that fight-or-flight overdrive.
Anti-inflammatory action: Chronic inflammation can mess with your cardiovascular system. Early research suggests tVNS has anti-inflammatory effects that might help your blood vessels respond better to position changes2.
Autoantibody reduction: Some people with orthostatic intolerance have antibodies that interfere with their cardiovascular regulation. Preliminary evidence indicates tVNS might help decrease these problematic autoantibodies3.
The bottom line? VNS appears to work on multiple levels to calm down an overactive autonomic nervous system.
Is Vagus Nerve Stimulation Different from Other POTS Treatments?
Most treatments for orthostatic intolerance focus on managing symptoms. Doctors might prescribe medications to increase blood volume, constrict blood vessels, or slow heart rate.
VNS takes a different approach. Instead of just treating symptoms, it aims to retrain your autonomic nervous system. The goal is to strengthen your body's natural ability to handle position changes.
And unlike medications, chronic tVNS appears to be well-tolerated in initial studies. Researchers haven't found major side effects in the short-term trials2.
Of course, this doesn't mean VNS replaces medical care. If you're dealing with dizziness or rapid heart rate when standing, you need a proper medical evaluation first. These symptoms can have serious underlying causes that require treatment.
What You Should Know About VNS for Standing Intolerance
The research on vagus nerve stimulation for orthostatic symptoms is encouraging. But it's also limited.
Most evidence comes from people with POTS specifically. We don't know yet how well it works for other forms of standing intolerance. And the studies are small and short-term.
In the studies that showed benefits, people typically used tVNS devices for 1-2 hours daily over 8 weeks, with electrodes placed on the ear. Some protocols involved shorter 30-minute sessions twice daily. The specific parameters varied between studies, but most used gentle electrical pulses at frequencies between 25-30 Hz.
If you're dealing with symptoms when you stand up, start with your doctor. They can rule out serious conditions and discuss whether approaches like vagus nerve stimulation might fit into your overall treatment plan.
Some people also find that improving their overall heart rate variability through vagus nerve support helps with orthostatic symptoms, though this connection needs more research.