Can VNS Improve Digestion? What Research Shows
That uncomfortable bloating after dinner? The sluggish feeling when food just sits in your stomach? The gut issues that flare up during stressful periods? These common digestive complaints might trace back to a single nerve that connects your brain to your belly. Vagus nerve stimulation may support digestive function by turning on your parasympathetic nervous system. This is your 'rest and digest' mode that controls gut movement, stomach acid, and brain-gut signals. Early research from 2024-2025 shows promise. But the science is still new12.
How Does the Vagus Nerve Control Digestion?
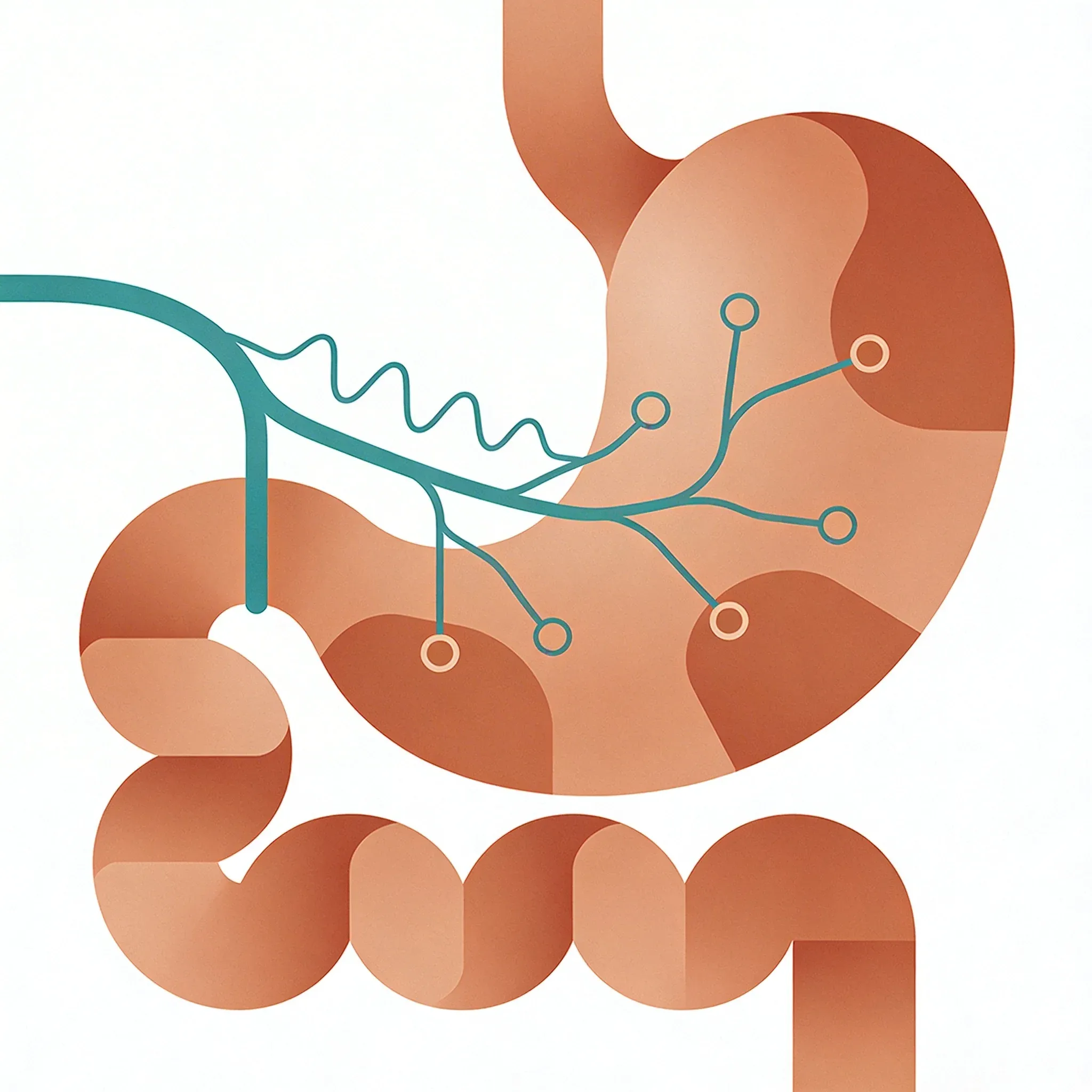
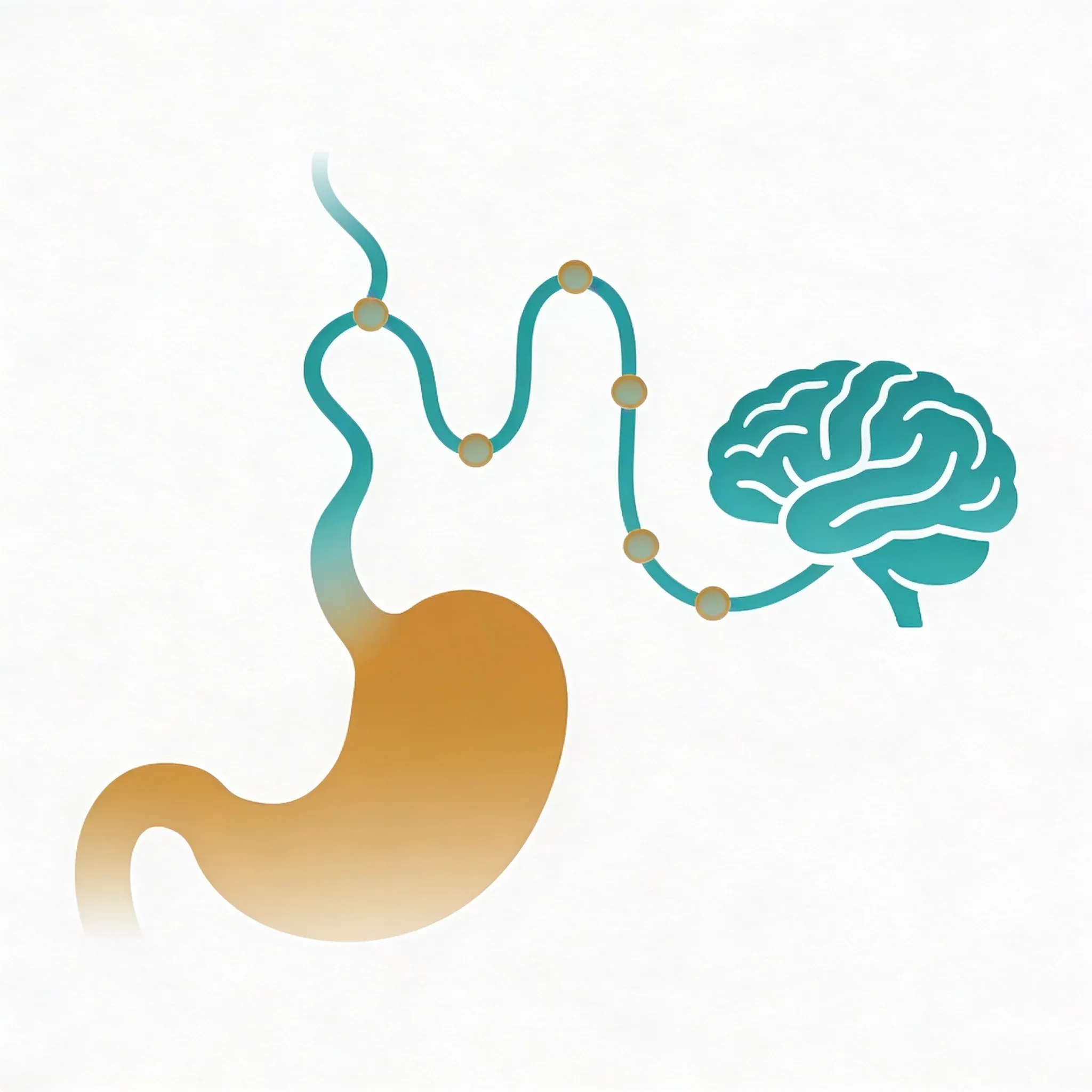
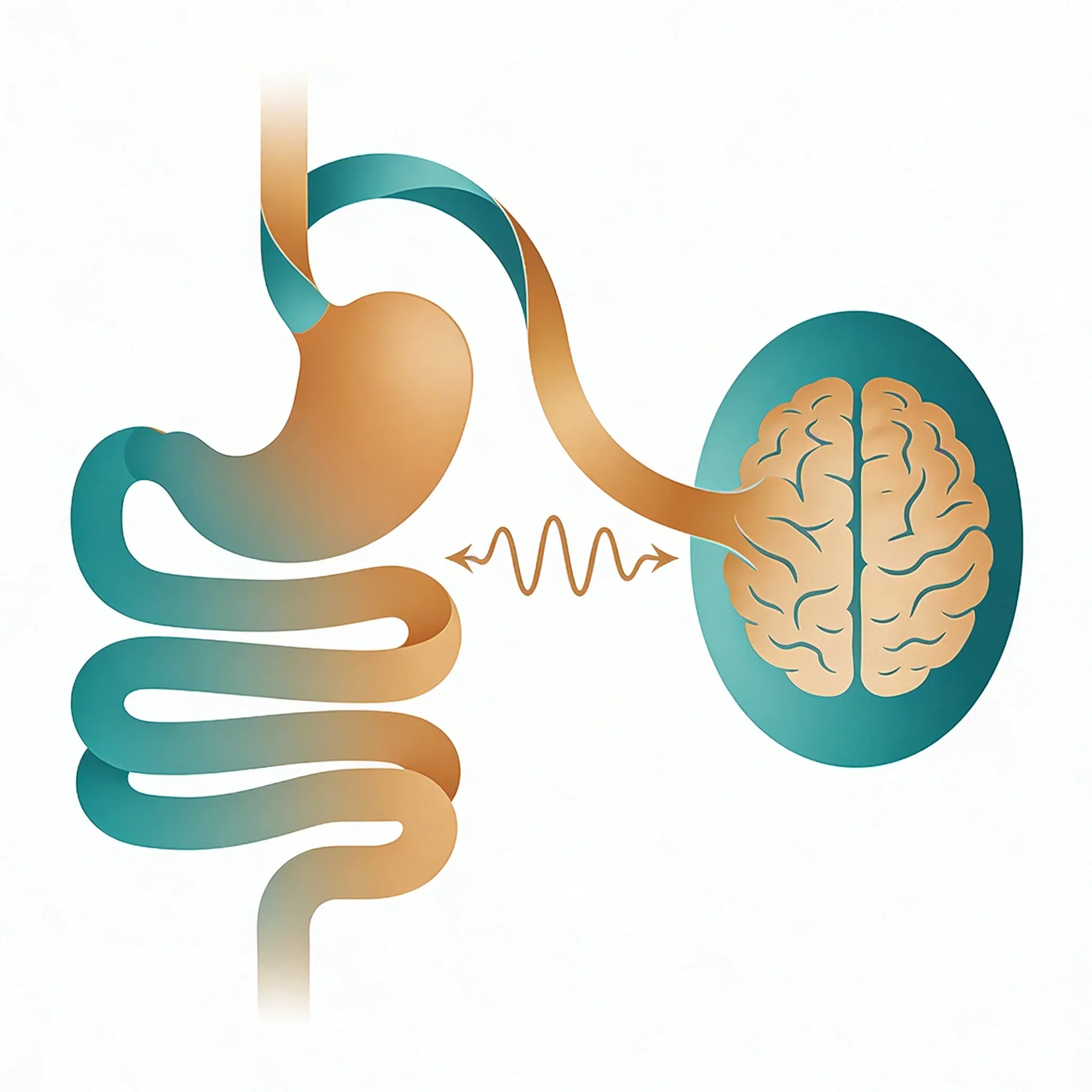
Your vagus nerve acts like a busy two-way street with constant traffic between your brain and gut. It carries signals that tell your stomach when to make acid. It tells your intestines when to move food along. And it tells your gut when to speed up or slow down.
When the vagus nerve fires, it releases acetylcholine. This chemical messenger works like a master key that unlocks specific digestive processes. Just as the right key opens only certain locks, acetylcholine fits into precise receptors throughout your digestive system. It unlocks stomach acid production, intestinal muscle contractions, and enzyme release - each process activated by this same molecular key fitting into its matching receptor1.
The connection works both ways. Your gut sends about 80% of vagus nerve signals upward to the brain. So when your digestive system struggles, your brain gets the message through this same neural highway.
What Does Research Show About VNS and Gut Health?
New studies suggest vagus nerve stimulation might influence digestion in several ways:
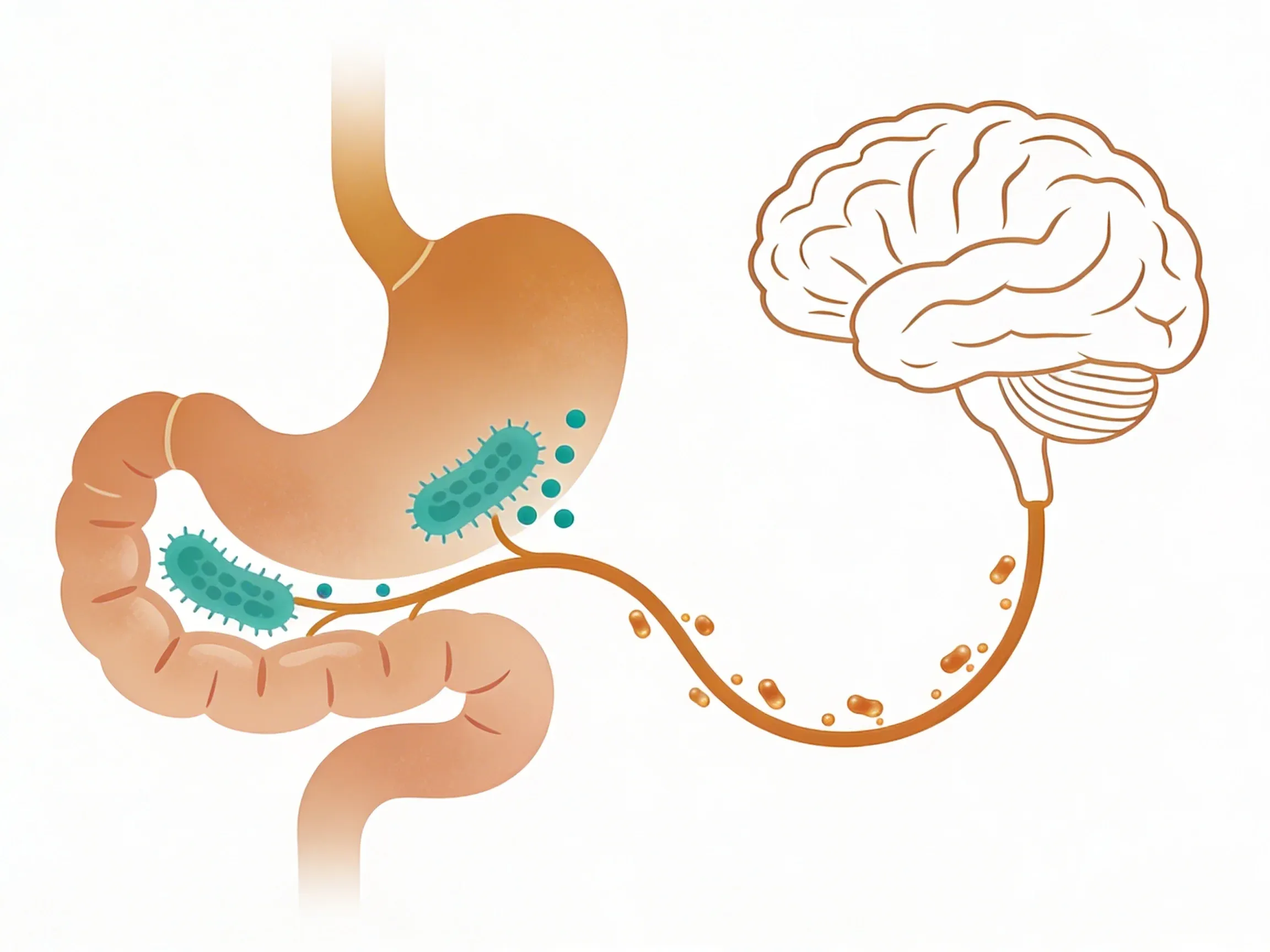
Gut bacteria balance: A 2025 review found that research suggests electrical stimulation may influence gut microbiota through direct electrical communication between nerve signals and bacteria. This means the nerve's electrical activity might directly affect the balance of microorganisms in your gut1.
Inflammation control: The vagus nerve turns on what researchers call the cholinergic pathway. This system may help calm intestinal inflammation. Early research suggests this could support digestive comfort. But more clinical trials are needed3.
Digestive reflexes: Some studies show vagus nerve activation might strengthen your gut's natural defense mechanisms. This could mean better protection against digestive irritation. But the clinical uses are still being studied2.
Here's the thing: most of this research is very recent. We're talking about studies published in 2024 and 2025. This means the findings need more validation before we can draw firm conclusions.
Can VNS Help With Specific Digestive Issues?
Some early research has looked at targeted digestive problems:
Acid reflux: A 2024 study used acupuncture targeting vagus nerve pathways for GERD. People showed reduced reflux symptoms and lower inflammatory markers. But this was acupuncture, not electrical stimulation. And the study was small4.
Gut motility: Research suggests when this nerve works well, food moves through your digestive tract more smoothly. Stimulation might support this natural process2.
Digestive inflammation: The anti-inflammatory effects of vagus nerve activation could help with conditions like inflammatory bowel disease. But research in this area is extremely early3.
The bottom line? Early signs are encouraging. But we don't have enough clinical evidence to recommend VNS as a treatment for specific digestive disorders.
What About Different Types of VNS?
Not all vagus nerve stimulation works the same way for digestion:
Breathing exercises: Slow, deep breathing naturally stimulates the vagus nerve through the diaphragm. This is the most accessible approach and has the best safety profile.
Cold exposure: Brief cold showers or face plunging can activate the vagus nerve through the dive reflex. This triggers the same parasympathetic response that promotes optimal digestive function - including increased stomach acid production and improved gut motility. Some people report digestive improvements, though this is mostly personal stories, not research.
Electrical devices: Transcutaneous VNS devices that clip to your ear deliver targeted stimulation. The research on these for digestion is very limited. Though they may offer more consistent activation than breathing exercises.
Implanted devices: Surgical VNS implants have been studied for severe digestive conditions in medical settings. This research doesn't necessarily apply to non-invasive consumer devices.
Remember: most of the promising digestive research involves medical-grade interventions or specific techniques like acupuncture. It doesn't necessarily apply to the consumer wellness devices available today.
How Might VNS Support Your Digestive System?
If you're considering vagus nerve approaches for digestive wellness, here's what current research suggests:
Stress reduction: We know stress disrupts digestion. Techniques that activate the vagus nerve and promote a sense of calm might help digestive function by turning on your parasympathetic nervous system. This is the mode where digestion works best.
Consistency matters: The vagus nerve responds to regular activation. This could be breathing exercises, cold exposure, or electrical stimulation devices. Daily practice might be more helpful than occasional use.
Individual responses vary: Some people might notice digestive changes within days or weeks of starting vagus nerve practices. Others might see no effect at all. The research hasn't identified who's most likely to respond.
Talk to your doctor before starting any new wellness practice. This is especially important if you have digestive disorders like GERD, IBD, or long-term gut issues. Vagus nerve stimulation isn't a replacement for medical treatment.