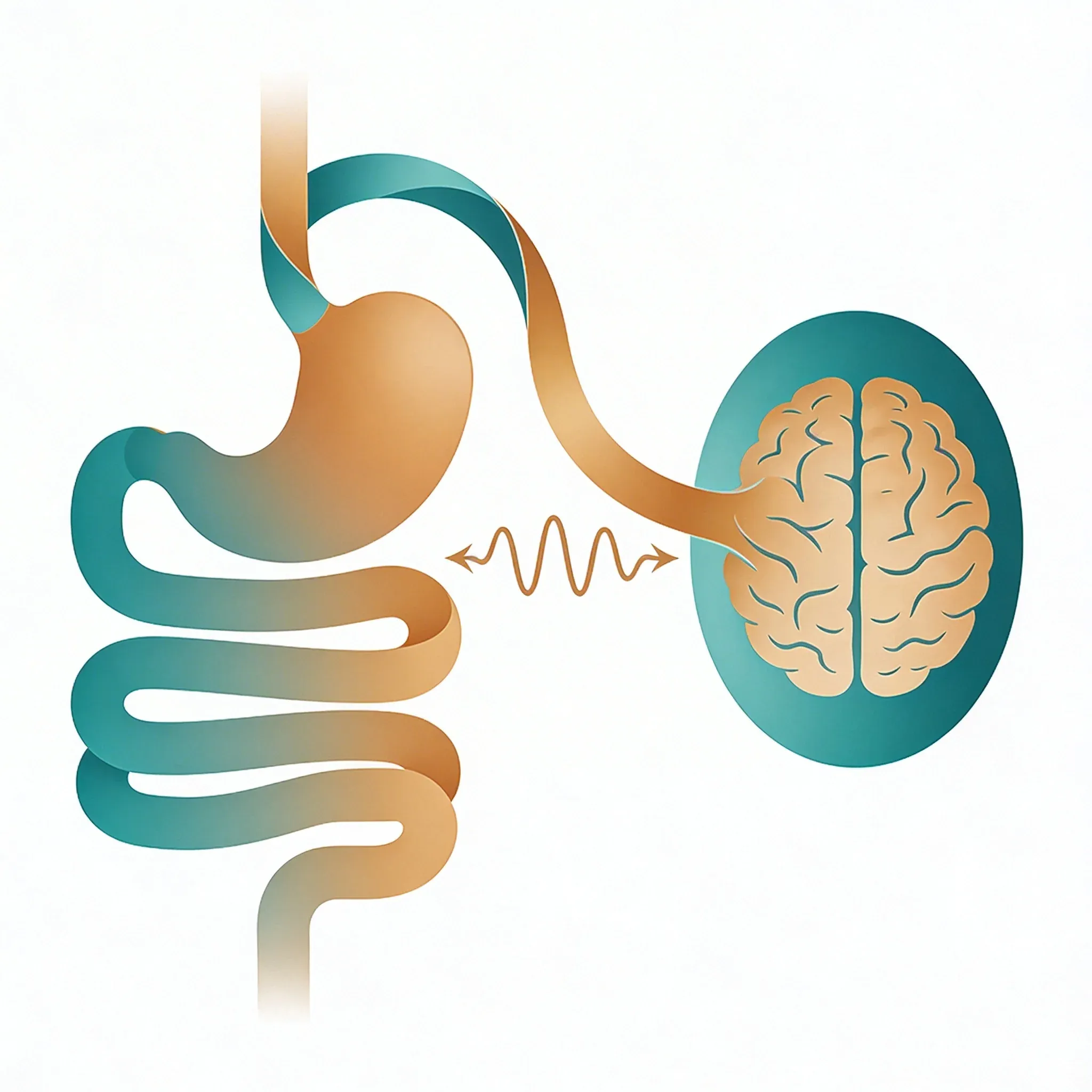
Your vagus nerve acts like a high-speed data cable between your gut and brain. It carries over 80,000 signals daily. About 80% of these messages travel upward -- from your digestive system to your brain. Only 20% flow downward1. This creates what scientists call the gut-brain axis. It's a communication network that affects everything from when you feel hungry to how stress hits your stomach.
What Is the Vagus Nerve Highway Between Gut and Brain?
Think of your vagus nerve as the body's longest phone line. It starts in your brainstem (an area called the medulla oblongata). It winds down through your neck, past your heart and lungs. It ends in your belly2.
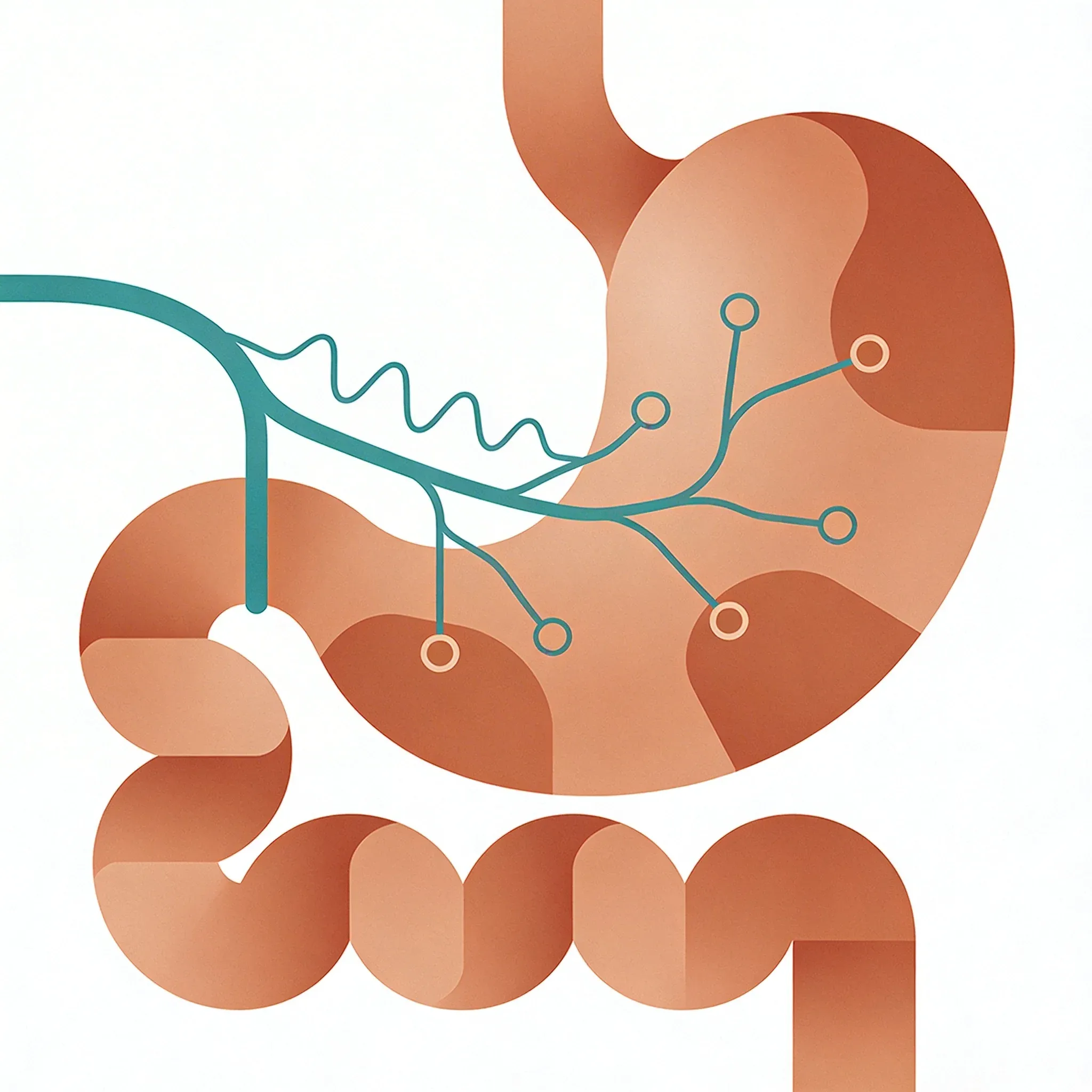
This isn't just one simple wire. The vagus nerve contains thousands of individual nerve fibers bundled together. Each fiber has a special job. Some detect chemical changes in your gut. Others sense when food arrives in your stomach. Still others monitor inflammation levels.
The nerve connects directly to major digestive organs:
- Your stomach (controlling acid production and movement)
- Your small intestine (managing nutrient signals)
- Parts of your colon (coordinating waste processing)
But here's what makes it amazing: most traffic flows upward. Your gut constantly reports to your brain about what's happening down below.
How Do Gut Signals Travel to Your Brain?
When you eat, your digestive system doesn't work alone. It starts sending status updates to your brain right away. It uses special sensors called vagal afferent neurons3.
These sensory neurons start from clusters of nerve cell bodies. These clusters are called nodose ganglia. They sit near your ears. From there, they send long projections down to your gut organs.
When these sensors detect changes, they fire messages back up to your brain. Changes like food arriving, pH shifts, or chemical signals from gut bacteria trigger these messages.
The signals travel at about 120 meters per second. That means a message from your stomach reaches your brain in roughly 100 milliseconds. That's faster than you can blink.
Here's what your gut reports to your brain:
- Physical changes: Stomach stretching when you eat. Intestinal muscle squeezes during digestion.
- Chemical signals: Nutrient levels, hormone releases, toxin detection
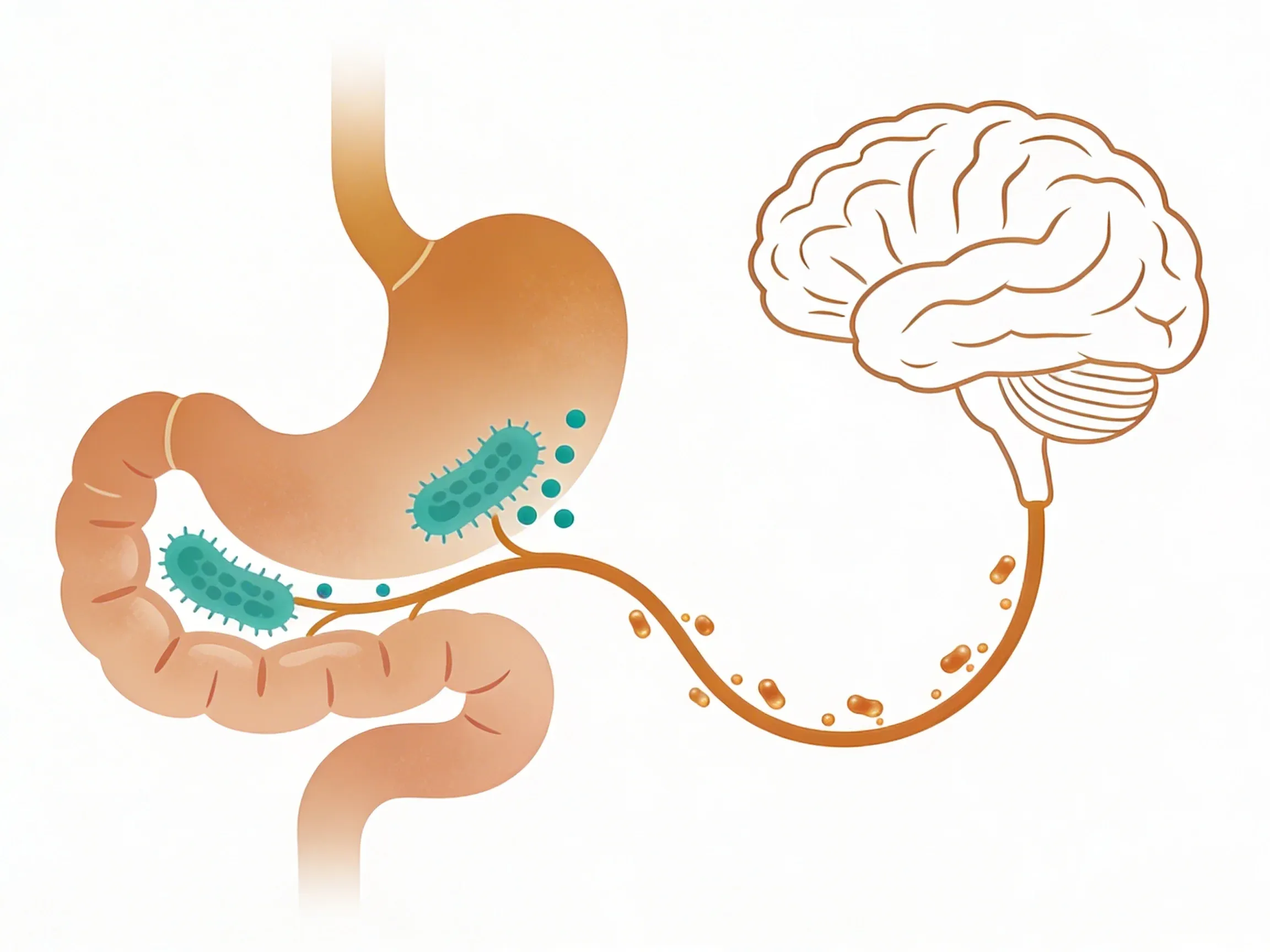
- Bacterial communication: Your gut microbes produce compounds that vagal sensors can detect
- Inflammation status: Immune activity levels in your digestive tract
Your brain takes in all this information. Then it decides how you should feel and respond.
How Does Your Brain Respond to Gut Messages?
Once your brain gets gut signals through the vagus nerve, it triggers responses. Some you notice. Some happen without your awareness.
You notice these sensations:
- Hunger and fullness
- Nausea or digestive comfort
- Food cravings
- That "gut feeling" during stress
These responses happen on their own:
Your brain sends signals back down the vagus nerve to coordinate digestion. These efferent (brain-to-gut) signals control stomach acid production. They manage digestive muscle squeezes. They trigger enzyme releases. It's like your brain acts as the conductor of your digestive orchestra.
But the vagus nerve doesn't work alone. It partners with your sympathetic nervous system, hormones, and immune signals. Together they create the complete gut-brain axis1. When you're stressed, your brain can slow digestion. It does this by reducing vagal activity to your gut.
This is why stress often causes stomach problems. Your brain tells your digestive system to pause operations. It waits until the perceived threat passes.
Can You Feel Your Vagus Nerve Working?
You can't directly feel nerve signals traveling. But you definitely experience the results. That satisfied feeling after a good meal? That's your gut sending "all good" signals to your brain via the vagus nerve.
The "butterflies" you get when nervous? That's your brain reducing vagal input to your stomach. This changes how your digestive muscles squeeze.
Some people are more sensitive to gut-brain communication than others. This might explain why certain people have stronger "gut instincts." It might also explain why some are more affected by digestive issues during stress.
Research suggests you can influence this communication. You can do this through practices that activate your vagus nerve. Examples include deep breathing techniques or specific stimulation methods that may help calm the nervous system and support healthy gut-brain signaling.
Why Does This Connection Matter for Your Health?
The gut-brain highway does more than manage digestion. This communication network affects:
Mood control: Your gut produces about 90% of your body's serotonin. Vagal pathways help transport mood signals from gut to brain2.
Immune responses: The vagus nerve helps coordinate anti-inflammatory responses. When your gut detects harmful bacteria, it can trigger brain-controlled immune reactions.
Stress recovery: Strong vagal tone supports better stress bounce-back. This partly happens through improved gut-brain communication.
Microbiome influence: Your gut bacteria can affect brain function through vagal pathways. Some helpful bacteria produce compounds that stimulate vagal sensors. This may affect mood and thinking4.
This explains why digestive health and mental health often go together. Problems with gut-brain communication may contribute to both digestive disorders and mood issues.
Actionable Ways to Support Your Gut-Brain Connection
You can try specific techniques that research suggests may help support healthy gut-brain communication:
Deep Belly Breathing: Breathe in slowly through your nose for 4 counts, allowing your belly to expand. Hold for 2 counts. Exhale through your mouth for 6 counts. Practice for 5-10 minutes daily, especially before meals.
Cold Water Face Immersion: Fill a large bowl with cold water (50-60°F). Immerse your face from temples to chin for 15-30 seconds. This may help activate the vagus nerve's parasympathetic response. Try 2-3 times per week.
Mindful Eating Practice: Eat one meal per day without distractions. Chew each bite 15-20 times. Focus on taste, texture, and how your body responds. This may help strengthen gut-brain awareness signals.
These techniques work by potentially supporting vagal tone and the relaxation response that aids healthy digestion.