How Your Vagus Nerve Controls Pain Signals in Your Brain
That nagging back pain that won't quit? The stomach cramping that flares with stress? The headaches that seem to have a mind of their own? Research suggests your vagus nerve may act as a natural pain control system that could help with these persistent problems. This major nerve sends signals that can reduce how much pain you feel. It connects directly to brain regions that process pain. It also triggers the release of chemicals like serotonin that naturally block pain signals1. This connection explains why some people find relief through vagus nerve activation.
How Does the Vagus Nerve Block Pain Signals?
When you feel pain, it travels through a complex network in your brain. This network is called the "pain matrix." Your vagus nerve works against this system.
Think of it like a volume dial on a stereo. The pain matrix turns up the volume on pain signals. Your vagus nerve turns it down by releasing natural chemicals that block pain transmission. When your vagus nerve activates, it floods key brain regions with serotonin and norepinephrine. These neurotransmitters act like acoustic dampeners in a recording studio. They absorb and muffle the pain signals before they reach your conscious awareness.
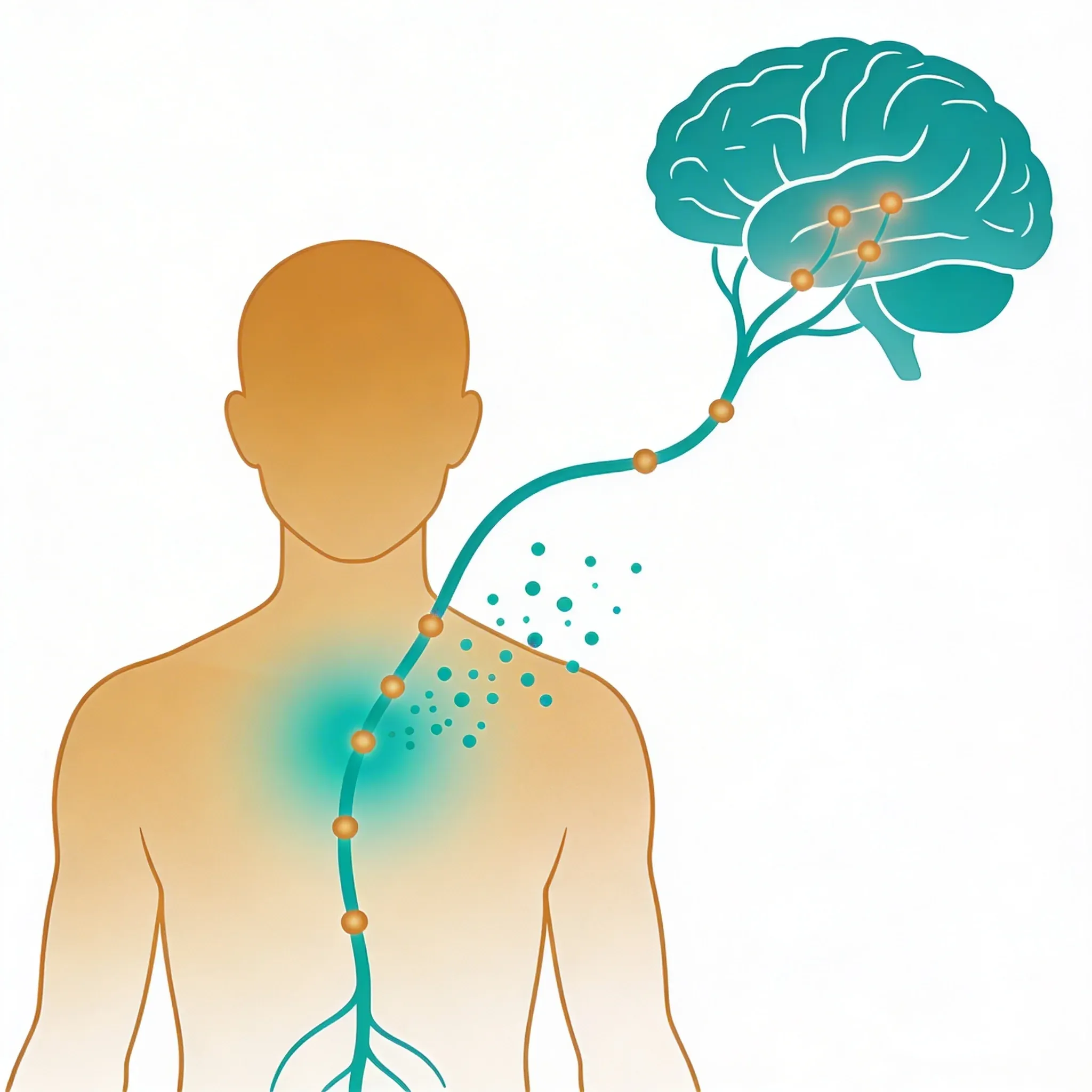
Here's how it works: Your vagus nerve carries sensory information to a brain region. This region is called the nucleus tractus solitarius. From there, signals spread to key areas that control pain perception. These include your amygdala, hippocampus, and anterior cingulate cortex1.
These connections help explain why stress makes pain worse. When your vagus nerve is underactive, your brain processes pain more intensely. When it's active, pain feels more manageable.
The vagus nerve also fights inflammation in your body. It reduces oxidative stress too. Since these processes fuel many types of long-term pain, reducing them can give relief at the source.
What Happens in Your Brain During Vagus Nerve Activation?
Stimulating your vagus nerve activates two key brain regions. These are the locus coeruleus and raphe nuclei. These areas pump out norepinephrine and serotonin. These are your body's natural pain-blocking chemicals1.
This is the same pathway that prescription antidepressants target. But your vagus nerve can trigger it naturally.
Research shows this system works fast. In one study of 48 healthy volunteers, something interesting happened. Just one hour of transcutaneous vagus nerve stimulation made people less sensitive to heat pain during testing2. Their pain thresholds increased measurably.
The vagus nerve also changes how different pain-processing brain regions talk to each other. It improves "functional connectivity" between areas like the anterior cingulate cortex and insula1. This doesn't just reduce pain intensity. It can improve your emotional response to pain.
That matters because long-term pain isn't just about physical signals. It's about how your brain interprets and reacts to those signals.
Why Does Stomach Pain Travel Through the Vagus Nerve?
Scientists recently mapped exactly how stomach pain reaches your awareness. The pathway has four steps. Your vagus nerve controls the first one3.
The signal starts in your stomach. It travels up the vagus nerve to the nucleus tractus solitarius. Then it moves to the lateral parabrachial nucleus. Next, it goes to the paraventricular thalamus. Finally, it reaches your prefrontal cortex where you become aware of the pain.
This discovery helps explain why gut issues often come with mood changes and brain fog. Your vagus nerve connects your digestive system directly to brain regions that control thoughts and emotions.
It also suggests why vagus nerve stimulation techniques might help with both physical gut pain and the mental stress that often comes with digestive problems.
Can Vagus Nerve Stimulation Boost Other Pain Treatments?
Early research suggests your vagus nerve might enhance your body's natural opioid system. It may also influence how prescription pain medications work in your brain1.
This doesn't mean vagus nerve stimulation replaces other treatments. But it might make existing treatments work better.
Some research points to vagus nerve activity affecting heart rate variability. This measure tracks the variation between heartbeats. Higher heart rate variability indicates better nervous system flexibility and stress resilience. When your vagus nerve is more active, your heart rate variability typically improves. This enhanced nervous system balance often translates to better pain management, as your body becomes more adaptable to stress and recovery cycles.
Here's the key insight: pain isn't just about damaged tissue. It's about how your nervous system processes and responds to signals. Your vagus nerve gives you some control over that process.
What Types of Pain Respond to Vagus Nerve Approaches?
Research is still emerging. But early studies focus on several types of pain:
- Inflammatory conditions where reducing inflammation helps
- Long-term pain that involves central sensitization (when your nervous system becomes oversensitive)
- Pain conditions linked to stress and emotional factors
- Digestive pain and discomfort
The common thread: conditions where calming your nervous system and reducing inflammation could help.
Keep in mind that most research uses medical-grade stimulation devices. These require professional supervision. Home approaches like breathing exercises and cold exposure work through similar pathways. But they have different intensity.
For home practice, try the 4-7-8 breathing technique for 5 minutes daily: breathe in for 4 counts, hold for 7, exhale for 8. For cold exposure, start with 30 seconds of cold water at the end of your regular warm shower. These simple approaches may help support your body's natural pain management systems.
Talk to your doctor before trying any new approach for long-term pain. Vagus nerve activation can support other treatments. But it shouldn't replace proper medical evaluation and care.