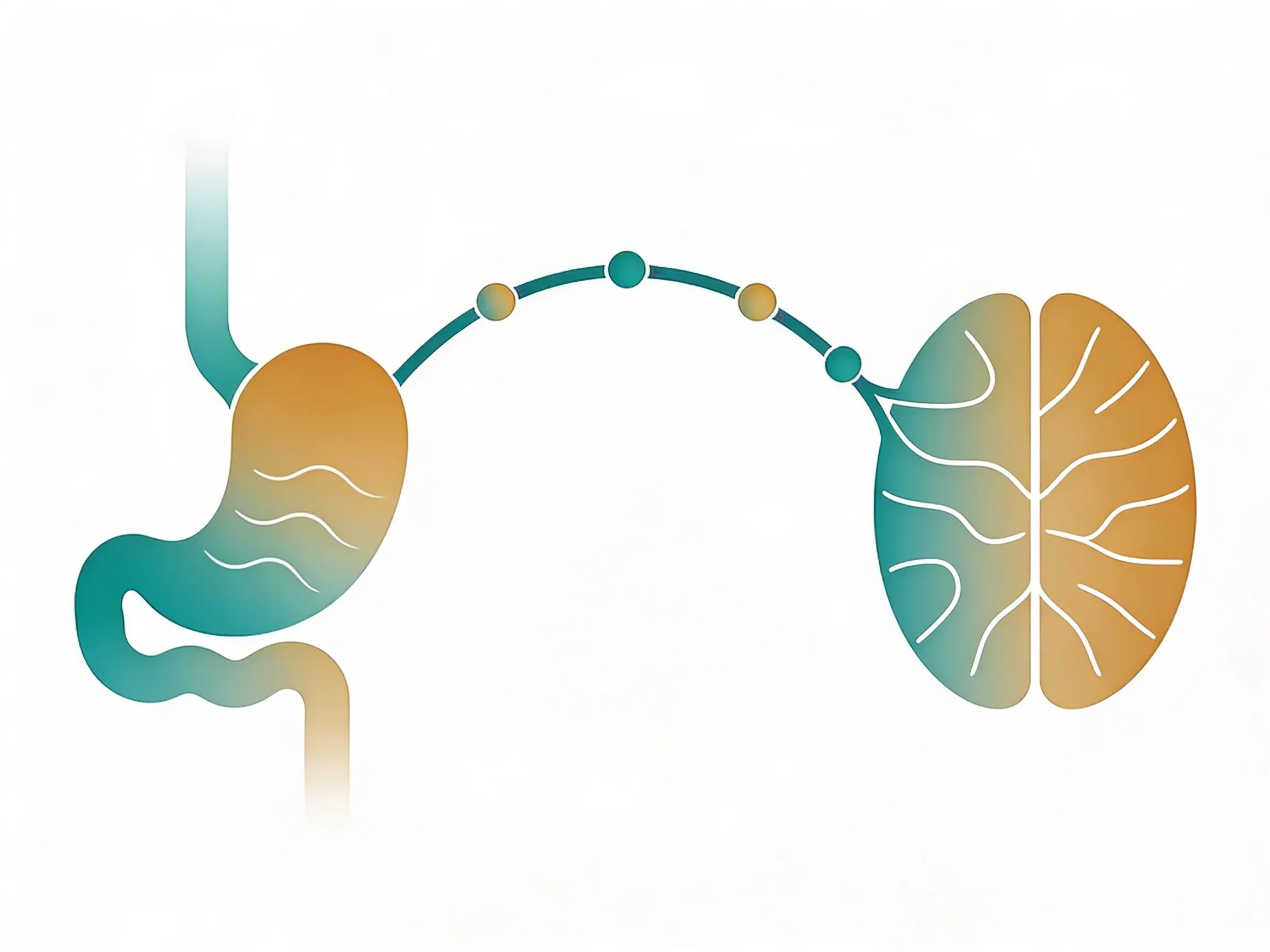
Your gut and brain are constantly chatting -- and your vagus nerve is the main phone line. This long nerve carries over 80,000 signals daily between your digestive system and brain, sharing information about everything from what you ate for lunch to how stressed you feel1. Most of these messages travel upward from gut to brain, not the other way around.
This connection explains why your stomach churns before a big presentation. Or why certain foods make you feel foggy. Your gut literally talks to your brain about how things are going down there.
What Is the Gut-Brain Connection?
The gut-brain axis is like a busy two-way highway. Your brain sends signals down to your gut about stress levels and emotions. Your gut fires back with updates about food, inflammation, and the trillions of bacteria living in your digestive tract.
Your vagus nerve handles most of this traffic. It's the longest cranial nerve in your body, running from your brainstem down to your abdomen. Think of it as the main communication cable between your two most important control centers.
But here's what's wild: your gut actually has its own "brain." The enteric nervous system contains over 500 million neurons -- more than in your spinal cord. This "second brain" works with your vagus nerve to keep digestion running smoothly, even when your main brain is busy with other things.
How Does the Vagus Nerve Carry Messages Between Gut and Brain?
Now that we understand the basic highway, let's look at the specific messages traveling in each direction. The vagus nerve works like a two-lane highway with traffic flowing in both directions.
Gut-to-brain signals travel on afferent fibers. These carry intel about:
- Nutrient levels and water status
- Digestive enzyme release
- Immune responses and inflammation
- Signals from your gut bacteria
Your gut is basically texting your brain all day: "We got protein down here." "Inflammation detected in sector 3." "The good bacteria are thriving."
Brain-to-gut signals travel on efferent fibers. These can:
- Reduce digestive inflammation
- Strengthen your intestinal barrier
- Adjust stomach acid production
- Speed up or slow down gut movement
When you're stressed, your brain tells your gut to hit the brakes on digestion. When you're calm, it gives the green light for optimal digestive function.
Can Your Gut Bacteria Actually Influence Your Brain?
With all these signals flying back and forth, you might wonder about the role of your gut bacteria in this communication network. Yes -- and this is where things get really interesting.
Your gut microbiome produces molecules that can directly activate your vagus nerve1. Think of your beneficial bacteria as tiny biochemical factories, each one churning out neurotransmitter-like compounds that hop onto the vagal highway and travel straight to your brain's control centers.
This means the health of your gut bacteria affects more than just digestion. Those trillions of microbes are sending chemical messages that can impact your mood, anxiety levels, and even decision-making.
Some research suggests this gut-brain communication through the vagus nerve plays a key role in anxiety-like behaviors2. When the vagal pathway from your gut is disrupted, it can affect how your brain processes emotional information.
Here's the thing: this research is still young. But it's pointing toward something remarkable -- your gut health and mental health are more connected than we ever realized.
What Happens When Gut-Brain Communication Goes Wrong?
So what happens when this sophisticated communication system breaks down? When vagal pathways between your gut and brain get disrupted, both systems can suffer.
You might experience:
- Digestive issues like bloating, irregular bowel movements, or food sensitivities
- Mood changes, increased anxiety, or brain fog
- Poor stress recovery
- Sleep disruptions
- Changes in appetite regulation
Chronic stress is a major disruptor. When you're constantly in fight-or-flight mode, your brain prioritizes survival over digestion. The vagal signals that normally keep your gut functioning smoothly get scrambled.
Inflammation is another culprit. When your gut is inflamed, it sends distress signals up the vagus nerve to your brain. Your brain interprets this as a threat and ramps up stress responses -- creating a cycle that's hard to break.
How Can You Support Healthy Gut-Brain Communication?
Fortunately, understanding this connection gives us practical ways to support both systems. Strengthening your vagus nerve function can improve the quality of gut-brain communication.
Breathing techniques directly stimulate the vagus nerve through your diaphragm. Slow, deep breaths tell both your brain and gut that it's safe to relax and digest.
Cold exposure activates the vagus nerve through what's called the dive reflex. Even splashing cold water on your face can trigger this calming response.
Certain foods support gut-brain health:
- Fermented foods feed beneficial bacteria
- Omega-3 fatty acids reduce inflammation along vagal pathways
- Fiber supports the gut microbiome
Some people explore vagus nerve stimulation techniques for more consistent support. The key is finding approaches that work with your lifestyle.
The bottom line? Your gut and brain are partners, not separate systems. Taking care of one helps the other.