How Your Vagus Nerve Acts as Your Body's Anti-Inflammatory Switch
Your vagus nerve works as a direct line between your brain and immune system. When inflammation starts in your body, this nerve spots it. Then it releases acetylcholine, a chemical that tells immune cells to dial down their activity.
This process is called the inflammatory reflex. It's your body's built-in system for stopping inflammation from getting out of control.
What Is the Inflammatory Reflex?
Think of the inflammatory reflex like a smoke detector linked to a sprinkler system. When your immune system spots a threat -- like an infection or tissue damage -- it releases inflammatory molecules called cytokines. These cytokines work like smoke signals.
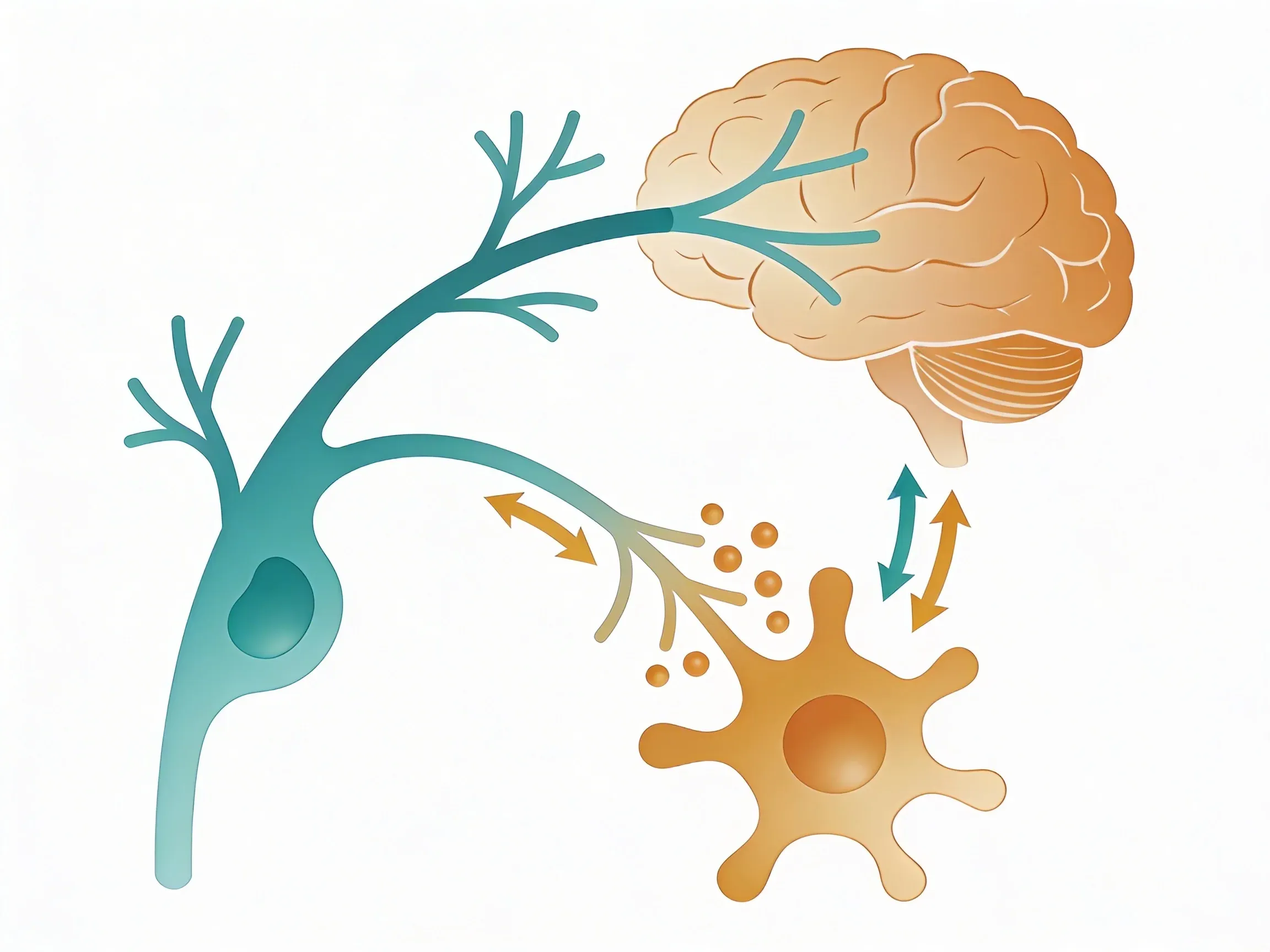
Your vagus nerve has special receptors that pick up these inflammatory signals. Once it detects them, the nerve sends a message to your brain. Picture your brain as a central dispatch center receiving these emergency calls.
This dispatch center (your brain) quickly evaluates the situation. Then it fires signals back down the vagus nerve -- like sending emergency responders to the exact location that needs help.
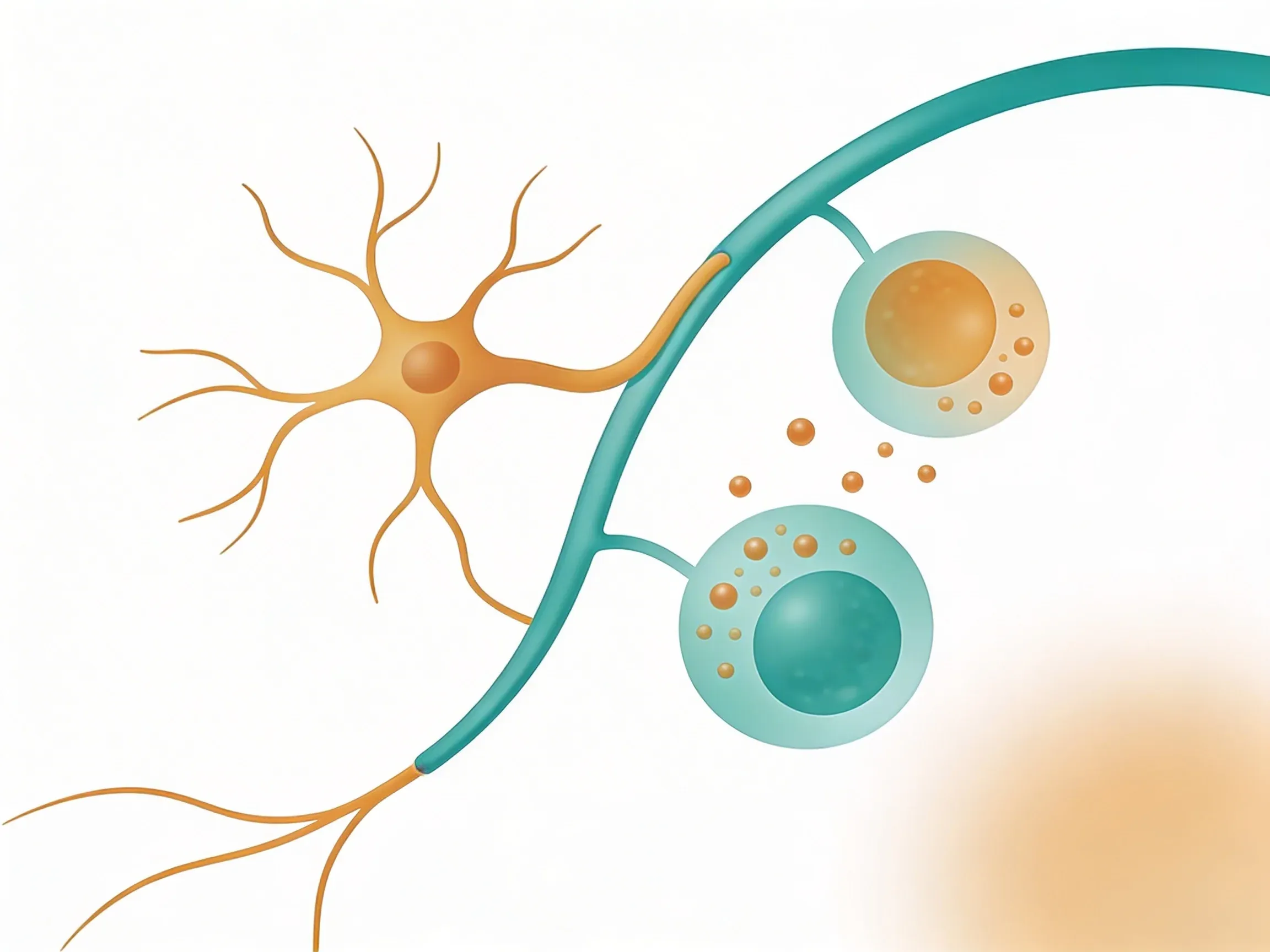
This return signal releases acetylcholine near immune cells. That's where the magic happens.
How Does the Anti-Inflammatory Pathway Work?
The anti-inflammatory pathway is the technical name for how your vagus nerve calms inflammation. Here's how it works step by step:
First, immune cells like macrophages release inflammatory cytokines when they meet a threat. These molecules create inflammation. That's helpful for fighting infections. But it can damage healthy tissue if it goes on too long.
Next, your vagus nerve detects these inflammatory signals through special receptors. It constantly watches your body's inflammatory status -- like a dispatch operator monitoring emergency calls across the city.
Then your brain processes this information. It decides if the inflammation level is right. If inflammation is getting too strong, your brain sends a signal back down the vagus nerve.
Finally, the vagus nerve releases acetylcholine near the immune cells. This chemical binds to specific spots called alpha-7 nicotinic receptors on macrophages and other immune cells.
When acetylcholine binds to these receptors, it's like hitting the brakes on inflammation. The immune cells reduce their production of inflammatory cytokines.
The whole process happens quickly -- within minutes of the first inflammatory trigger.
Why Your Brain Needs Real-Time Inflammation Control
Inflammation is a double-edged sword. You need it to fight infections and heal injuries. But too much inflammation for too long can damage healthy tissue. It can contribute to long-term health problems.
Your vagus nerve acts as the highway between your immune system and your brain. Without this connection, your brain would be flying blind when it comes to managing inflammation.
Think of your brain as the central command center coordinating responses across your entire body. When inflammation flares up in your gut, your brain's dispatch center needs that information immediately. It can then coordinate the right response and send help where it's needed most.
Key takeaway: Your immune system is spread throughout your entire body. It needs a way to work together. The vagus nerve provides that coordination.
When inflammation starts in your gut, your brain needs to know about it. The inflammatory reflex makes sure information travels both ways. From the gut to the brain. And from the brain back to the gut.
What Happens When This System Gets Disrupted?
When the inflammatory reflex doesn't work right, inflammation can become long-term. Your immune system keeps making inflammatory signals. But your vagus nerve can't tell it to calm down well enough.
This breakdown is associated with various inflammatory conditions according to research. Studies show that people with reduced vagal tone often display elevated inflammatory markers and increased risk of chronic inflammatory diseases. The body loses its ability to control immune responses properly.
People with reduced vagal tone -- meaning their vagus nerve doesn't work well -- often show higher levels of inflammatory markers in their blood. Their inflammatory reflex isn't as responsive.
The opposite is also true. Research indicates that people with higher vagus nerve tone tend to have better inflammatory balance. Their bodies are better at turning inflammation on when needed. And off when the threat is gone.
Several factors can affect how well your inflammatory reflex works:
- Long-term stress can suppress vagal function and disrupt inflammatory control
- Poor sleep interferes with the vagus nerve's ability to regulate immune responses
- Aging naturally reduces vagal tone, which may explain why inflammation tends to increase with age
- Certain lifestyle factors like regular exercise and stress management can support healthy vagal function
Supporting Your Body's Natural Anti-Inflammatory System
While the inflammatory reflex is automatic, you can support its function through lifestyle choices. Anything that improves vagal tone helps this system work better.
Deep breathing exercises activate the vagus nerve and may support the inflammatory reflex. Try the 4-7-8 technique: inhale for 4 counts, hold for 7, exhale for 8. Practice this for 5-10 minutes twice daily.
Cold exposure also stimulates vagal activity. Start with 30-second cold showers and gradually work up to 2-3 minutes. Or try cold water face immersion for 15-30 seconds.
Research suggests that regular meditation can improve vagal tone over time. Aim for 10-20 minutes of daily meditation, focusing on mindfulness or loving-kindness practices.
Some people explore vagus nerve stimulation (VNS) devices to support this system. VNS involves electrical stimulation that may help strengthen the inflammatory reflex pathway. When considering approaches for using VNS for calming inflammation, it's important to understand timing and safety considerations.
Quality sleep is crucial too. Your vagus nerve needs enough rest to function properly. Poor sleep can disrupt the inflammatory reflex. It can lead to higher baseline inflammation.
The Bigger Picture of Inflammation Control
The inflammatory reflex represents one of the most elegant examples of mind-body connection in human biology. Your nervous system and immune system aren't separate. They're in constant communication.
Like a well-coordinated emergency response system, your brain's dispatch center works around the clock. It monitors inflammatory signals from throughout your body. Then it sends precise instructions back to keep everything in balance.
This discovery has changed how researchers think about inflammation and immunity. Instead of viewing inflammation as something that just happens at the tissue level, we now understand it's actively managed by your brain through the vagus nerve.
Understanding this pathway doesn't replace proper medical care for inflammatory conditions. But it does highlight why supporting vagal health through lifestyle choices makes sense for overall wellness.
Here's the thing: your body already has smart systems for managing inflammation. The inflammatory reflex is proof that your nervous system is designed to maintain balance. Not just in your thoughts and emotions. But in your immune responses too.
Talk to your doctor before starting any new wellness practice, especially if you have ongoing inflammatory health concerns.