How Your Vagus Nerve Controls Digestion (And Why It Matters)
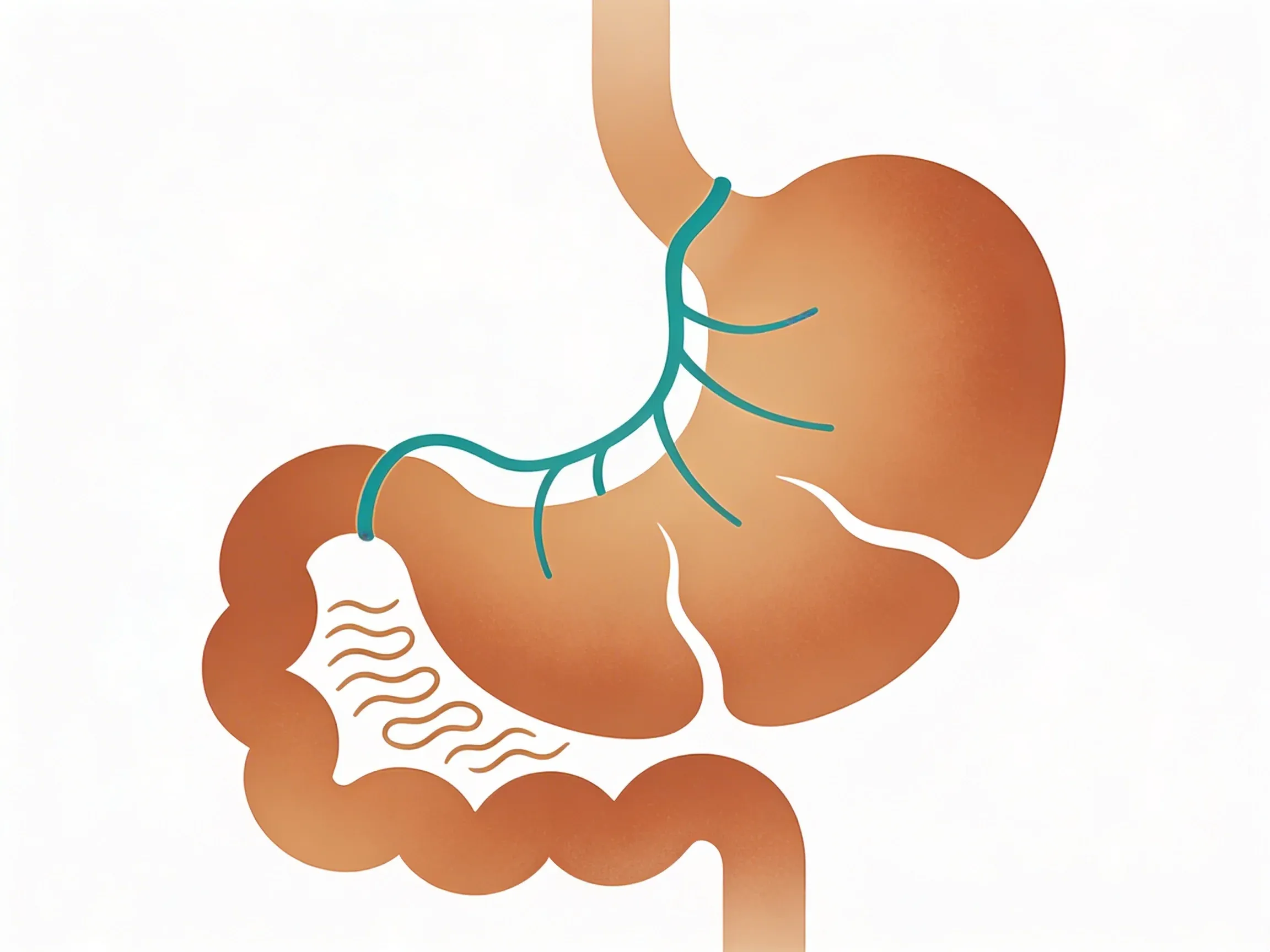
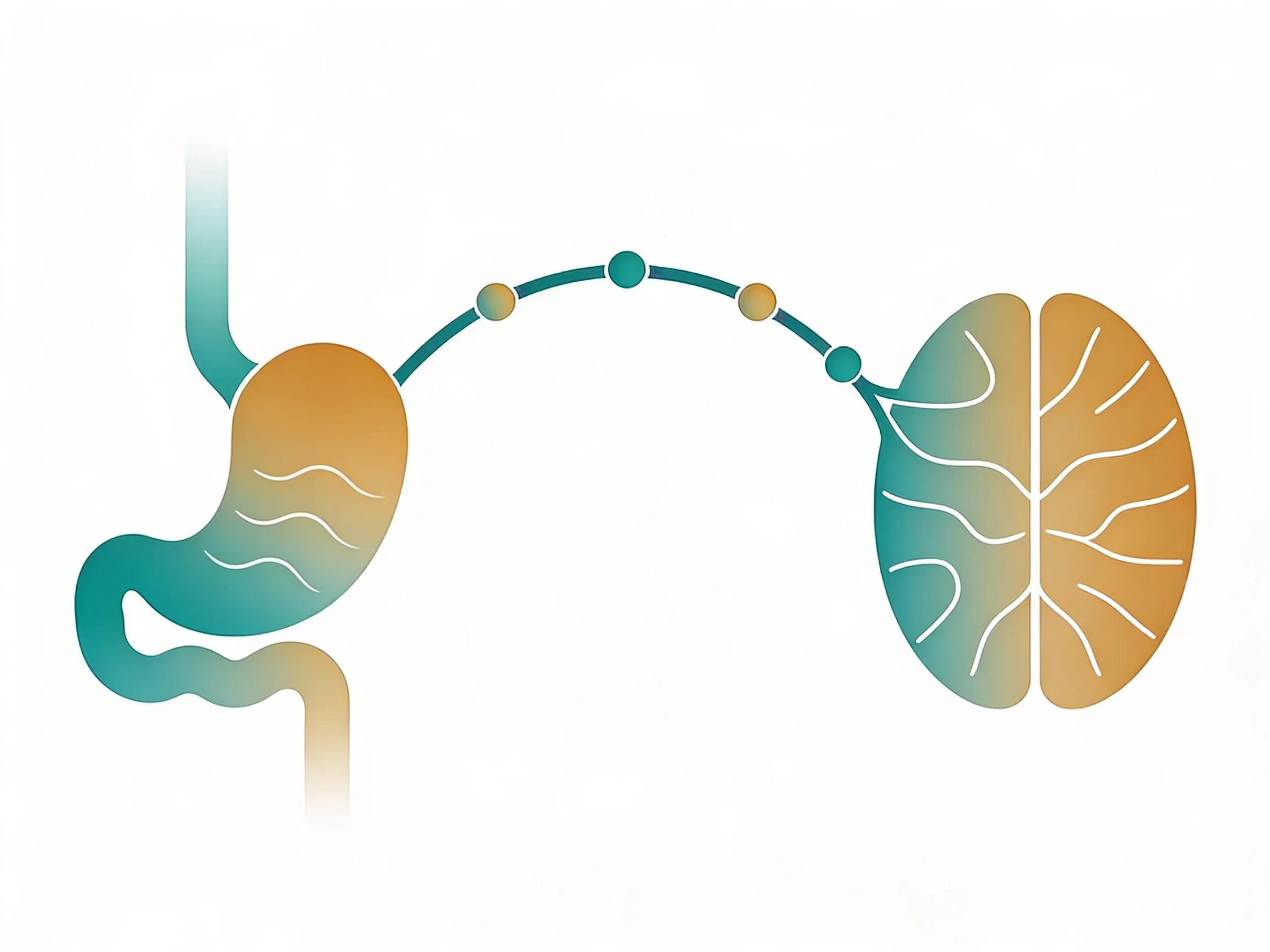
That heavy, uncomfortable feeling after eating when you're stressed isn't in your head. It's your vagus nerve -- the longest cranial nerve in your body that runs from your brainstem down to your belly. Research shows the vagus nerve plays a key role in controlling stomach acid production, muscle contractions that move food through your gut, and the signals that tell you when you're full1. When stress disrupts this connection, your digestion pays the price.
Why Does Stress Shut Down Your Digestion?
Here's the thing: your vagus nerve can only turn on digestion when your body feels safe.
When you're stressed, your sympathetic nervous system takes control. This "fight or flight" mode shuts down non-essential functions -- including digestion. Your vagus nerve literally cannot activate digestive processes during stress2.
Think of it like a sophisticated control tower at an airport. During normal conditions, the vagus nerve acts as an air traffic controller, coordinating two-way communication between your brain and gut. Signals flow down from brain to digestive organs ("start producing acid"), while status reports flow back up ("stomach is 80% full"). But when stress hits, it's like declaring an emergency that grounds all flights. The control tower goes silent, and digestive coordination shuts down completely.
This is why eating during stress leads to poor digestion, bloating, and discomfort. Your body isn't equipped to process food when it thinks you're in danger.
How Does the Vagus Nerve Actually Control Digestion?
Your vagus nerve controls digestion through a sophisticated two-way communication system.
The efferent fibers (signals going from brain to gut) tell your stomach to:
- Release digestive enzymes and stomach acid
- Contract muscles to mix and move food
- Coordinate the timing of digestive processes1
Meanwhile, afferent fibers (signals going from gut to brain) send information about:
- What nutrients are present in your digestive tract
- How full your stomach is
- Whether digestion is proceeding normally
This creates a feedback loop. Your gut tells your brain what's happening. Your brain adjusts digestive function accordingly.
What Happens in Your Stomach When the Vagus Nerve Activates?
When your vagus nerve fires, research suggests it triggers a cascade of digestive activity.
First, it signals your stomach to release gastric acid and digestive enzymes. These break down proteins and prepare nutrients for absorption.
Then it activates unique mixing motions called segmentation. These aren't just simple contractions. They're coordinated movements that thoroughly mix food with digestive juices3.
The vagus nerve also controls gastric emptying. This is how quickly food moves from your stomach to your small intestine. It coordinates this timing with over 30 different digestive hormones to ensure optimal nutrient absorption1.
How Does Your Vagus Nerve Know When You're Full?
Your vagus nerve acts like a nutrient sensor.
As you eat, mechanoreceptors in your stomach wall detect stretching. Chemical receptors identify specific nutrients in your digestive tract. Both send signals up the vagus nerve to your brainstem1.
This information travels to the dorsal motor nucleus of the vagus. This is a control center that processes satiety signals. When you've had enough, this area reduces digestive stimulation. It sends "full" signals to your conscious brain.
But here's what most people miss: this system only works properly when your vagus nerve is functioning well. Poor vagal tone can disrupt hunger and fullness cues. The key question becomes: how can you support this natural communication system?
Can You Improve Vagal Control of Digestion?
The good news? You can support healthy vagal function through simple practices that help activate your parasympathetic nervous system.
Deep breathing exercises activate your parasympathetic nervous system. This helps shift your body into "rest and digest" mode. Even a few slow, deep breaths before eating can improve digestive function. Understanding when to use specific breathing techniques for calm can help you time these practices optimally around meals for better digestive support.
Building on these breathing techniques, cold exposure is another practice that may help support vagal function. Brief cold exposure -- like cold showers or ice baths -- can stimulate the vagus nerve and potentially improve its overall tone. However, it's best to avoid cold exposure immediately before or after meals, as the stress response from cold might temporarily interfere with digestive processes.
Some people also find that vagus nerve stimulation devices help maintain consistent parasympathetic activation. But more research is needed on their specific effects on digestion.
The key is creating the right internal environment for your vagus nerve to do its job.
What About Digestive Problems and Vagus Nerve Dysfunction?
Poor vagal function shows up in digestion in several ways.
Reduced stomach acid production can lead to difficulty breaking down proteins. It can also affect absorbing nutrients. Delayed gastric emptying might cause bloating and discomfort after meals. Disrupted satiety signals can affect appetite regulation2.
Some research suggests that improving heart rate variability may support better digestive function overall. HRV is a marker of vagal tone.
But it's important to understand the limits here. Supporting vagal function may help with general digestive comfort. But persistent digestive issues need professional evaluation. Conditions like gastroparesis, SIBO, or inflammatory bowel disease need medical treatment.
The Bottom Line on Vagus Nerve and Digestion
Your vagus nerve is the master coordinator of your digestive system. It controls acid production, muscle contractions, nutrient sensing, and satiety signals. But it only works when your body feels safe enough to digest.
This is why managing stress matters so much for gut health. It's also why practices that activate your vagus nerve may support better digestive function. These include deep breathing or targeted stimulation.
The research on vagus nerve-gut communication is expanding rapidly. We're learning that this connection runs much deeper than before understood. It has implications for everything from nutrient absorption to mood regulation.