How Your Vagus Nerve Acts as Your Body's Inflammation Controller
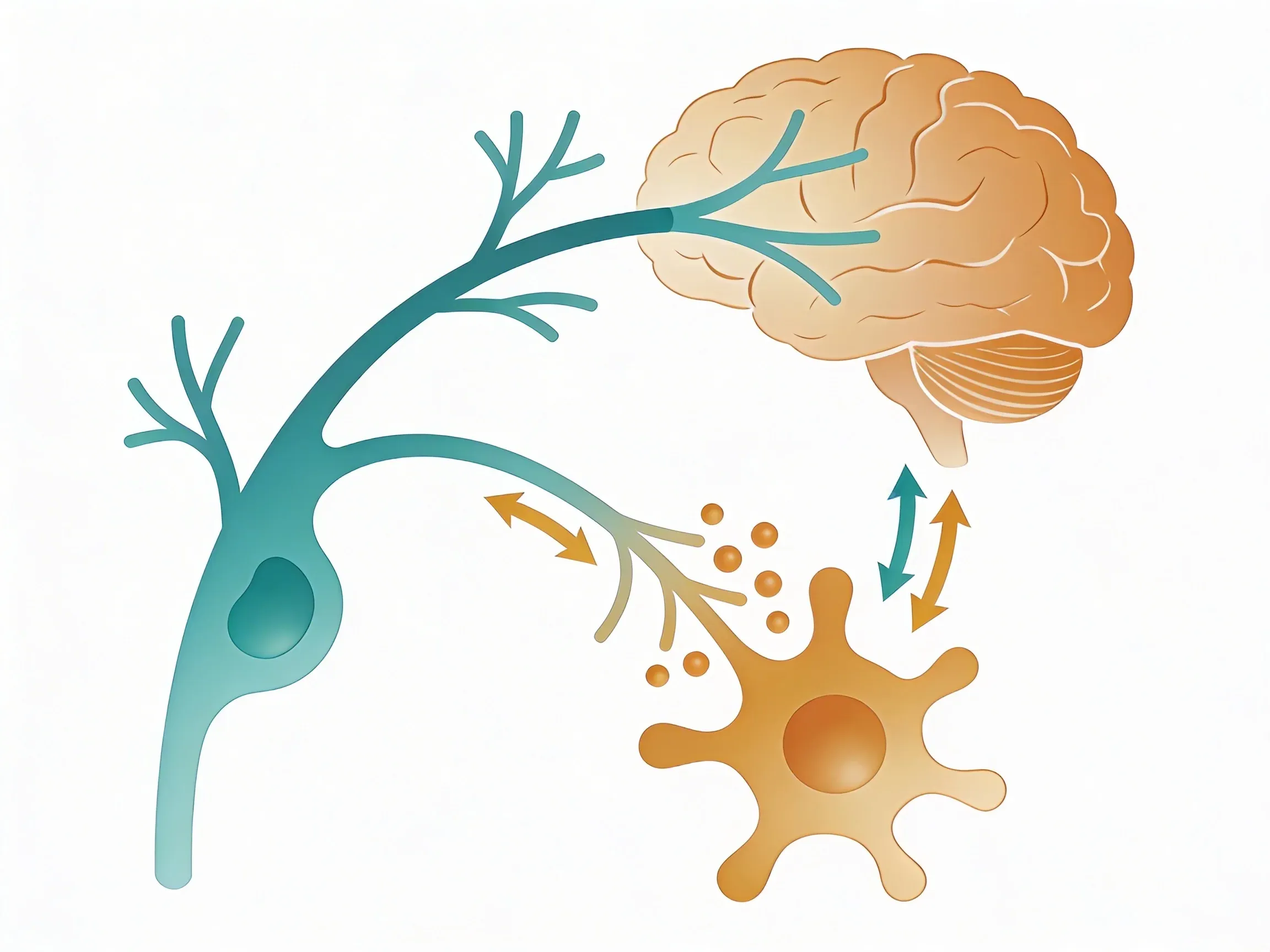
Your vagus nerve contains specialized sensors that detect inflammatory molecules called cytokines as they circulate through your body. When it spots trouble, it sends rapid signals back to immune organs to dial down excessive inflammation. This two-way communication system, called the inflammatory reflex, acts like a built-in thermostat for your immune system1.
What Are Cytokines and Why Do They Matter?
Cytokines are chemical messengers that immune cells use to communicate. Think of them as text messages between your white blood cells.
Some cytokines ramp up inflammation to fight infections or heal injuries. Others cool things down once the threat passes. The balance matters because too much inflammation damages healthy tissue. Too little leaves you vulnerable to infections.
During severe illness, this balance can tip dangerously. A "cytokine storm" floods the body with inflammatory signals. Your immune system attacks everything in sight, including your own organs.
That's where your vagus nerve steps in as a safety switch.
How Does Your Vagus Nerve Detect Inflammation?
Your vagus nerve runs from your brainstem to your abdomen, with branches touching your heart, lungs, liver, and gut. Along this pathway sit specialized sensory neurons that work like molecular detectors2.
These neurons recognize specific cytokines:
- TNF-α (a major inflammation driver)
- IL-1β (signals tissue damage)
- IL-10 (an anti-inflammatory messenger)
Different nerve clusters respond to different cytokines. Your brain gets distinct reports about what type of immune activity is happening and where3.
Here's the clever part: your vagus nerve doesn't just monitor inflammation. It actively controls it.
What Happens When Your Vagus Nerve Spots Trouble?
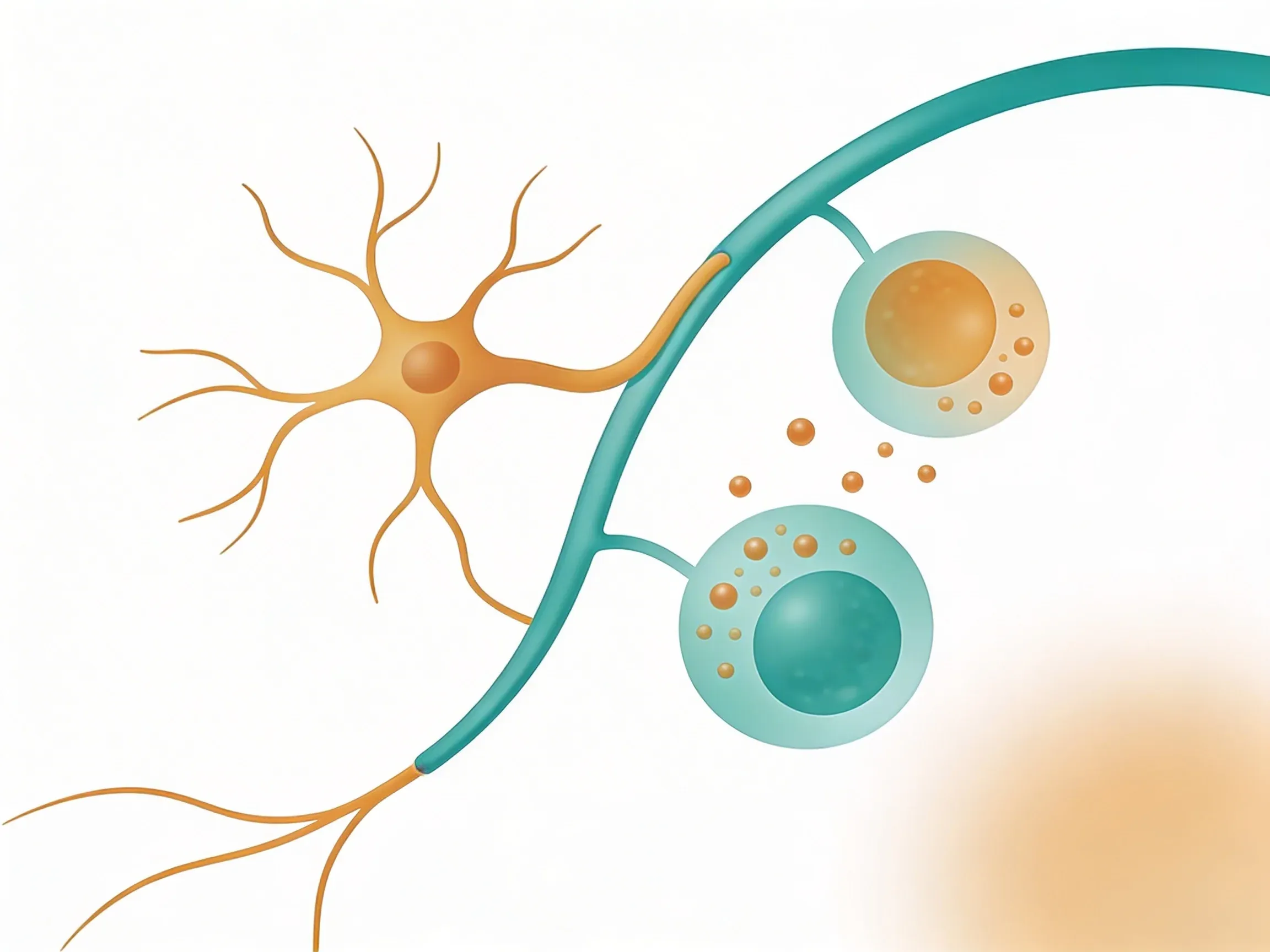
Once vagal sensors detect cytokines or bacterial toxins, they fire signals up to your brainstem. Your brain processes this immune intelligence and decides how to respond.
If inflammation is ramping up too fast, your brain sends commands back down the vagus nerve. These outgoing signals use a chemical called acetylcholine to communicate with immune organs.
The spleen gets the message first. Acetylcholine tells immune cells there to stop pumping out inflammatory cytokines. The liver and gut receive similar "calm down" signals1.
This happens in minutes, not hours. It's faster than hormonal responses and more precise than drugs.
Researchers call this the inflammatory reflex because it works automatically, like pulling your hand away from a hot stove.
Can Vagus Nerve Stimulation Help Control Inflammation?
Early research suggests that stimulating the vagus nerve can reduce inflammatory cytokines. In laboratory studies, electrical vagus nerve stimulation lowered TNF-α levels during artificial inflammation4.
This doesn't mean vagus nerve stimulation is a treatment for inflammatory diseases. The research is still experimental. Most studies use animal models or test tubes, not humans with real conditions.
But the basic principle makes sense. If your vagus nerve naturally regulates inflammation, supporting its function might help maintain immune balance.
Practical Approaches to Support Vagal Function
Some people try specific protocols to support vagal tone:
- 4-7-8 breathing: Inhale for 4 counts, hold for 7, exhale for 8. Practice 5 minutes twice daily, ideally in the morning upon waking and evening before bed
- Cold exposure: End showers with 30-60 seconds at 50-60°F water temperature. Start with morning exposure to boost alertness. Note: avoid if you have heart conditions or are pregnant
- Box breathing: 4 counts in, 4 hold, 4 out, 4 hold, repeated for 5 minutes. Best practiced during evening wind-down routines
Most people report subtle improvements in stress tolerance and recovery within 2-3 weeks of consistent practice. More noticeable changes in overall resilience may take 6-8 weeks of regular application.
Others use devices that deliver gentle electrical stimulation to vagus nerve pathways. Understanding when to use VNS for calm can help determine if such approaches might be appropriate for your situation.
What Goes Wrong When This System Fails?
During chronic inflammation, your vagus nerve's ability to regulate cytokines becomes impaired. The nerve fires more often at baseline but responds less precisely to specific threats2.
Think of it like a smoke detector with a dying battery. It might go off randomly but miss real fires.
This breakdown may contribute to autoimmune diseases, where the immune system attacks healthy tissue. It might also explain why some people develop long-lasting inflammation after infections.
The connection between vagus nerve dysfunction and cytokine storms in human disease is still being studied. We know the pathway exists, but researchers are still mapping how it goes wrong in different conditions.
The Bottom Line?
Your vagus nerve is more than a relaxation pathway. It's an active participant in immune regulation, constantly monitoring and adjusting inflammatory responses.
This research opens new questions about supporting immune health through nervous system care. While we're still learning how to apply this knowledge clinically, understanding the connection helps explain why nervous system health affects immunity.
If you're dealing with chronic inflammation or autoimmune issues, work with healthcare providers who understand both your immune system and nervous system. The two are more connected than we once realized.