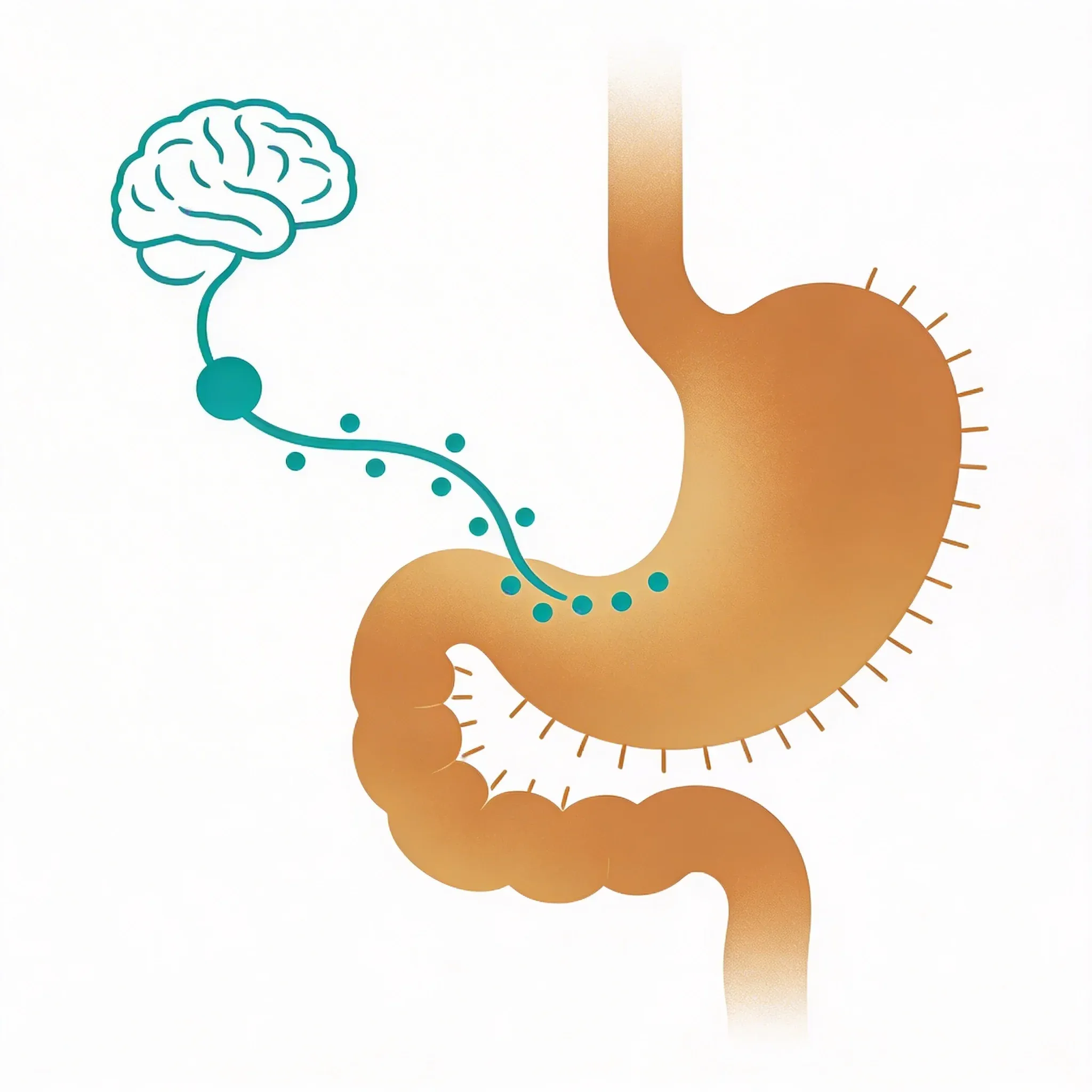
How Your Vagus Nerve Fights Gut Inflammation (And Why It Matters)
Ever notice how stress hits your stomach first? That knot in your gut during a presentation, the digestive chaos after bad news—there's real science behind this gut feeling. Early research suggests your vagus nerve may help reduce harmful molecules like tumor necrosis factor (TNF) in your gut. It also helps maintain your intestinal barrier integrity. This prevents gut leakage issues that can trigger inflammation throughout your body1.
What Is the Vagus Nerve's Role in Gut Health?
Think of your vagus nerve as a smart home security system that continuously monitors for threats and deploys targeted countermeasures. When inflammation sensors detect danger in your gut, the system doesn't just sound an alarm—it analyzes the specific threat, encodes that information into precise neural signals, then dispatches customized anti-inflammatory responses to exactly where they're needed.
When your vagus nerve detects inflammatory signals in your digestive tract, it responds in two main ways. First, it activates your body's natural stress response system to release cortisol. This dampens inflammation. Second, it uses direct nerve-to-nerve communication called vagovagal reflexes to quickly calm inflamed tissues1.
Your vagus nerve also communicates with the trillions of bacteria in your gut. It does this through special cells called enteroendocrine cells and enteric neurons. These cells likely use serotonin-based mechanisms to relay information between your gut microbiome and your brain2.
This connection explains why digestive issues often come with mood changes. And why stress can trigger gut problems.
How Does Vagal Inflammation Control Actually Work?
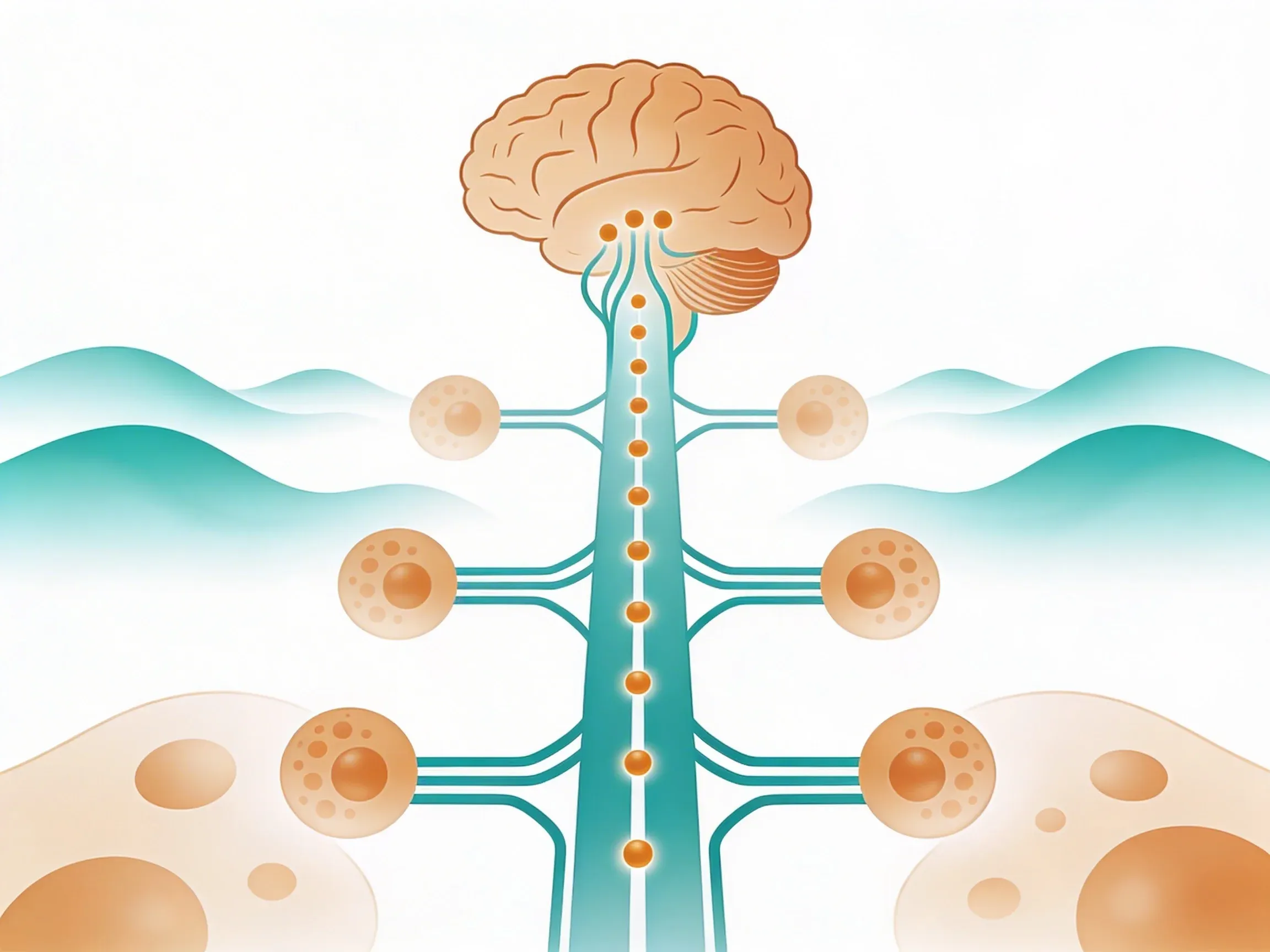
Your vagus nerve contains special sensory neurons that act like tiny inflammation detectors. These neurons can sense inflammatory molecules like TNF and IL-1 released by immune cells in your gut. When they detect these signals, they encode the information with distinct neural patterns. Then they send it straight to your brain3.
Here's the clever part: your brain doesn't just receive this inflammation alert. It sends anti-inflammatory instructions right back down the vagus nerve. These signals target the inflamed area. They reduce the production of harmful inflammatory molecules.
The vagus nerve helps maintain what researchers call intestinal barrier integrity. Your gut lining acts as a selective filter. It lets nutrients through while blocking toxins and bacteria. When this barrier becomes too permeable (sometimes called "leaky gut"), inflammatory substances can escape into your bloodstream. This causes problems throughout your body.
Your vagus nerve helps keep this barrier strong and selective.
Can Poor Vagal Function Increase Gut Inflammation?
Yes, and the triggers might surprise you. Poor diet, long-term stress, and infections can all disrupt your vagal signaling. They throw off your gut bacteria balance2. When this happens, your gut's natural anti-inflammatory defenses weaken.
Stress is particularly damaging to the gut-brain connection. When you're stressed for a long time, your sympathetic nervous system (fight-or-flight mode) stays active. This suppresses your vagus nerve's calming influence. This creates a cycle: stress increases gut inflammation. This sends more inflammatory signals to the brain. Which creates more stress.
Signs that your vagus nerve may not be supporting your digestive health well include:
- Frequent bloating or digestive discomfort
- Irregular bowel movements
- Food sensitivities that seem to worsen with stress
- Digestive issues that flare during stressful periods
Of course, these symptoms can have many causes. If you have ongoing digestive problems, talk to your doctor about proper evaluation and treatment.
What Can Support Your Vagus Nerve and Gut Health?
Early research suggests several approaches may help support the vagus nerve's anti-inflammatory effects in the gut. Deep breathing exercises that emphasize long, slow exhales can activate your vagus nerve. Try 4-7-8 breathing (inhale 4, hold 7, exhale 8) practiced for 5-10 minutes daily. They shift your nervous system toward the rest-and-digest mode that supports healthy digestion.
Some people find that specific techniques for using vagus nerve stimulation during calm moments help them manage stress-related digestive discomfort before meals or during stressful periods.
Cold exposure, like brief cold showers, may also activate anti-inflammatory pathways and potentially support gut health. The cold triggers a stress response that, when brief, can strengthen vagal tone. This improved nerve function may help the gut better regulate inflammatory responses by enhancing the nerve's ability to detect and respond to gut-based inflammation signals.
Interesting research is emerging on gut-directed therapies like hypnotherapy for conditions like irritable bowel syndrome and inflammatory bowel disease. These approaches may work partly by supporting vagal function through relaxation-induced activation of the parasympathetic nervous system, which includes the vagus nerve's anti-inflammatory pathways2.
Here's the thing: while the research on vagus nerve and gut health is promising, most studies are still early stage. More human trials are needed to fully understand how we can best support this brain-gut connection.
Key takeaway: Your vagus nerve doesn't just help with digestion -- it actively protects your gut from inflammation and maintains the delicate balance that keeps your digestive system healthy.